 Integrated post-cardiac arrest care is the 5th link in the AHA adult chain of survival. Topics of focus for post-cardiac arrest care include temperature control, hemodynamic and ventilation optimization, immediate coronary reperfusion with PCI (percutaneous coronary intervention), glycemic control, neurologic care and other technical interventions. To be successful, post-cardiac arrest care requires an integrated multidisciplinary approach.
Integrated post-cardiac arrest care is the 5th link in the AHA adult chain of survival. Topics of focus for post-cardiac arrest care include temperature control, hemodynamic and ventilation optimization, immediate coronary reperfusion with PCI (percutaneous coronary intervention), glycemic control, neurologic care and other technical interventions. To be successful, post-cardiac arrest care requires an integrated multidisciplinary approach.
For the purposes of this site, the review of post-cardiac arrest care interventions will focus primarily on immediate post-arrest interventions and aspects that you will most likely be tested on.
For a complete review of the subject refer to your AHA provider manual. (pages: 150-158)
Temperature Control
Temperature control which was previously called TTM (targeted temperature management) is the only intervention that has been shown to improve neurological outcomes after cardiac arrest. Temperature control should occur soon after ROSC (return of spontaneous circulation) for all cardiac arrest patients, and should be maintained for 36 hours. The decision point for the use of temperature control is whether or not the patient can follow commands. (lack of meaningful response to verbal commands)
Temperature control includes choosing one temperature between 32-37.5 °C (89.6-97.5 °F) and then holding that temperature for at least 36 hours. Common methods used for maintaining temperature control are endovascular catheter, surface cooling devices, or other simple surface cooling interventions.
During induced temperature control, the patient’s core temperature should be monitored with any one of the following: esophageal thermometer, a bladder catheter in the nonanuric patients, or a pulmonary artery catheter if one is already in place.
Axillary and oral temperatures are inadequate for monitoring core temperatures.
Ventilation Optimization
During the post-cardiac arrest phase, inspired oxygen should be titrated to maintain an arterial oxygen saturation of ≥90-98%. The goal is to avoid hypoxia and hyperoxia. This reduces the risk of oxygen toxicity. Excessive ventilation should also be avoided because of the potential for reduced cerebral blood flow related to a decrease in PaCO2 levels. Also, excessive ventilation should be avoided because of the risk of high intrathoracic pressures which can lead to adverse hemodynamic effects during the post-arrest phase.
Quantitative waveform capnography can be used to regulate and titrate ventilation rates during the post-arrest phase. Visit the link for more details about waveform capnography.
Avoid excessive ventilation. Ventilation should start at 10/min and should be titrated according to the target PETCO2 of 35-45 mmHg.
Hemodynamic Optimization
Hypotension, a systolic blood pressure < 90 mmHg should be treated and the administration of fluids and vasoactive medications can be used to optimize the patient’s hemodynamic status. While the optimal blood pressure during the post-cardiac arrest phase is not known, the primary objective is adequate systemic perfusion, and a mean arterial pressure of ≥ 65 mmHg should accomplish this. A mean arterial pressure ≥ 65 mmHg should be maintained during the post-cardiac arrest phase.
The goal of post-cardiac arrest care should be to return the patient to a level of functioning equivalent to their prearrest condition.
IV infusions for the control of post-arrest hypotension:
- IV Fluid Bolus: Give 1-2 L of normal saline or LR
- Epinephrine 2-10 mcg/min
- Dopamine 5-20 mcg/kg/min
- Norepinephrine 0.1-0.5 mcg/kg/min
Other considerations
Moderate glycemic control measures should be implemented to maintain glucose levels within a normal range, and since there is an increased risk for hypoglycemia, attention should be focused on prevention. No specific glycemic target range is recommended at this time.
Every effort should be made to provide coronary reperfusion (PCI), and interventions should be directed with this goal in mind. PCI has been shown to be safe and effective in both the alert and comatose patient, and hypothermia does not contraindicate PCI.
Click below to view the Post-Cardiac Arrest Algorithm Diagram. When finished, click again to close the diagram.
Post-Cardiac Arrest diagram
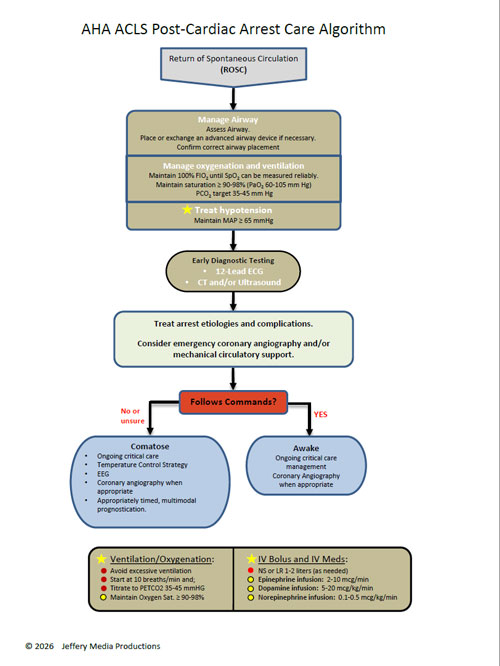
or Download the High Resolution PDF Here. (This will open in another window.)
Vesna Humo says
Hi Jeff, easier way to calculate mg/dL in mmol is amount of BS in mg divide with 18. Simple like that!:)
Best regards
Nancy Brady says
Jeff
Greetings.. Can you define mean arterial,pressure?
Thanks
Nancy
Jeff with admin. says
MAP, or mean arterial pressure, is defined as the average pressure in a patient’s arteries during one cardiac cycle. It is considered a better indicator of perfusion to vital organs than systolic blood pressure (SBP). True MAP can only be determined by invasive monitoring and complex calculations; however it can also be calculated using a formula of the SBP and the diastolic blood pressure (DBP).
This is typically calculated by automatic blood pressure machines and is shown like this 122/82 (96). The MAP is in parentheses
To calculate a mean arterial pressure, double the diastolic blood pressure and add the sum to the systolic blood pressure. Then divide by 3. For example, if a patient’s blood pressure is 83 mm Hg/50 mm Hg, his MAP would be 61 mm Hg. Here are the steps for this calculation:
MAP = SBP + 2 (DBP)
3
MAP = 83 +2 (50)
3
MAP = 83 +100
3
MAP = 183
3
MAP = 61 mm HG
Another way to calculate the MAP is to first calculate the pulse pressure (subtract the DBP from the SBP) and divide that by 3, then add the DBP:
MAP = 1/3 (SBP – DBP) + DBP
MAP = 1/3 (83-50) + 50
MAP = 1/3 (33) + 50
MAP = 11 + 50
MAP = 61 mm Hg
Reference
Kind regards,
Jeff
Annette Boyle says
Just sat acls in one of my learning stations my pt after rosc had sinus brady with low b/p and i was gonna give atropine .5mgs first before an infusion of dopamine and was told no go infusions after rosc .in another my pt had fast monomorphic vt low b/p after rosc and i was going to cardiovert told not correct .Im afraid i got upset and now feel
Like an idiot and nevet got the answer
Jeff with admin. says
First of all it’s sad that “learning stations” would be used to make someone feel like an idiot. These are supposed to be learning stations. You should not feel like an idiot, but should learn from the experience.
On to your concerns:
AHA Guidelines state that atropine would be the first medication of choice for symptomatic bradycardia.
On the other hand, there are many providers that go directly to transcutaneous pacing or the use of chronotropic agents like dopamine and epinephrine.
Technically, American Heart Guidelines would indicate atropine to be administered prior to these other infusions and transcutaneous pacing.
The second instance where you had monomorphic ventricular tachycardia in the post arrest phase, there would be a couple of variables that would be important to know. What was the BP after ROSC? Was the pt. conscious or unconscious? Also,
was the rhythm truly ventricular tachycardia or was it a wide complex tachycardia?
Was this learning station for an American Heart Association ACLS provider course? Or was this for some other type of certification?
Kind regards,
Jeff
Lenin Moreno says
What are the guidelines for Nutrition Support on patients on hypothermia?
I haven’t been able to find clear and concise information.
Jeff with admin. says
Any guidelines this would be beyond the scope of ACLS and are not covered by the AHA ACLS guidelines. I am not aware of any clear nutritional guidelines directed specifically toward targeted temperature management (therapeutic hypothermia).
Kind regards,
Jeff
davedani777@gmail.com says
where can I get more information about TTM GUIDELINES.Do you recommend any site
Jeff with admin. says
You can find a full review of TTM guidelines here: TTM ECC Guidelines Kind regards, Jeff
umeshyash says
Dear Jeff
In the acls manual at page no 19 it mentions that end tidal carbon dioxide PETco2 of 30 to 40 mm of Hg or Paco2 of 35 to 45 mm of Hg . But in Page no 146 it says that PET co2 of 35-40 mm 0f Hg or a P aco2 of 40-45 mm of Hg. which one is correct.
Jeff with admin. says
During the post cardiac arrest phase, ventilations should be titrated to achieve a PETCO2 of 35-45 mm Hg. This is the correct titration level for PETCO2. I’m not sure why AHA had this discrepancy in the provider manual. PETCO2 of 35-40 mm Hg in the post-arrest phase is correct.
Kind regards,
Jeff
davedani777@gmail.com says
Jeff
during the ACLS Training Mega code practice, one of the candidates asked the core temperature of the patient and the instructor said 36 degree celcius. Then the candidate opt for infusing normal saline ,not cold one. My doubt is if patient’s temperature is between 32-36, then cold saline infusion for inducing TTM can be avoided or not? Iam confused because every now and then I hear candidates asking for patient’s temperature before inducing TTM with cold saline even if the patient is unresponsive.Plz clarify my doubt
Jeff with admin. says
It would be ok to infuse cold saline especially if it was on the high side nearer to 36 deg. C.
It would be ok to not give the cold saline, however, it would not be contraindicated and it would be wise to include other measures to ensure that the temp is maintained below 36 deg. C.
Kind regards,
Jeff
mohammed Olofi says
Thanks for you, I understood more than in the last times.
ounworried@hotmail.com says
Thank you for the site. l am finding it very helpful l recertify in a week and reading the manual has proved boring. The interactive learning has made it do able.
Is it necessary to still read the manual after using this site especially with a week left to exam
how much is 144-180mg/dl in mmol/litre thats the units used here locally.
Regards
Ottilia
Jeff with admin. says
There are many health care providers how only use the site to prepare for the AHA ACLS Provider course. The feedback that I get is all very positive and I am confident that the site will thoroughly prepare you for the course.
The conversion from mg/dl to mmol/l would be 8 -10 mmol/l
Here is the conversion calculator that I used. Conversion Calculator
Kind regards,
Jeff
Yuvraj Singh Rathore says
My Brother is still neither fully concious nor pupilary reflections are there in eyes ever after passing of 103 days after Cardiac arrest. He is opening the eyes only. Resoonse is also there on Pain.Vitals are normal.
Pl guide how much more time he wil take for full recovery.
Jeff with admin. says
I don’t normally answer personal medical questions on this website because this website is designed to provide education for health care providers. You health provider should be able to answer this question for you. I can provide you with my opinion. I think that It is very unlikely that your brother will have any further recovery given the length of time that has already passed since the initial cardiac arrest. Kind regards, Jeff
Loomie07 says
Love this site. It makes learning enjoyable!
rhstanfordjr says
I am a current Paramedic student and the question arose as to why there is a difference in the epi drip (0.1-0.5 mcg/kg/min, page 73 AHA manual) when the patient is hypotensive. Can you provide any links as to why AHA has chosen this dosage for Epi?
Roger
Jeff with admin. says
AHA uses weight based dosing for the control of post-arrest hypotension because epinephrine used for post arrest hypotension is a much higher dose than that used for pacing in symptomatic bradycardia.
For instance, if you are treating a 70 kg adult for hypotension post arrest the dose of 0.1-0.5 mcg/kg/min will be 7-35 mcg per minute.
If you are treating any adult for symptomatic bradycardia with epinephrine your dose will be 2-10 mcg/min.
This is a big difference in dosing especially at the higher end.
AHA uses weight based dosing for the control of post-arrest hypotension because epinephrine used for post arrest hypotension is a much higher dose than that used for pacing in symptomatic bradycardia.
For instance, if you are treating a 70 kg adult for hypotension post arrest the dose of 0.1-0.5 mcg/kg/min will be 7-35 mcg per minute.
If you are treating any adult for symptomatic bradycardia with epinephrine your dose will be 2-10 mcg/min.
This is a big difference in dosing especially at the higher end.
I’m not sure if this answers your question, but here is a link to the AHA circulation journal section on Post-Cardiac Arrest.
Kind regards,
Jeff
Kind regards,
Jeff
DVK2485 says
Best learning ever. Used this site 2 years ago. Understood so much more than I had in the past. Thank you
Kriss says
So far, really like this site. Thankyou. Easy to navigate and comprehennsive. I work in a unit that thankfully does not have very many incidences to use ACLS but the potential is always there of course. Our hospital tries to have occassional drills for each dept to practice. I take my recert in a week and I’m a little less nervous each time and I have found your site very helpful for review and I don’t mind paying a few bucks to help you keep it going. Bless you.
Jeff with admin. says
So glad that the site has been helpful and thank you for the encouragement. Kind regards, Jeff
marcia gray says
Thank-you.