 Asystole is defined as a cardiac arrest rhythm in which there is no discernible electrical activity on the ECG monitor. Consequently, it is sometimes referred to as a “flat line.” Confirmation that a “flat line” is truly asystole is an important step in the ACLS protocol.
Asystole is defined as a cardiac arrest rhythm in which there is no discernible electrical activity on the ECG monitor. Consequently, it is sometimes referred to as a “flat line.” Confirmation that a “flat line” is truly asystole is an important step in the ACLS protocol.
Ensure that asystole is not another rhythm that looks like a “flat line.” Fine VF can appear to be asystole, and a “flat line” on a monitor can be due to operator error or equipment failure.
The following are common causes of an isoelectric line that are not asystole: 1. loose or disconnected leads; 2. loss of power to the ECG monitor; 3. low signal gain on the ECG monitor.
Asystole for many patients is the result of a prolonged illness or cardiac arrest, and prognosis is very poor. Few patients will likely have a positive outcome and successful treatment of cardiac arrest with asystole will usually involve the identification and correction of an underlying cause of the asystole.
The H’s and T’s of ACLS should be reviewed to identify any underlying cause that could have precipitated the asystole.
Some of the most common reasons to stop or withhold resuscitative efforts are:
- DNR status
- Threat to the safety of rescuers
- Family or personal information such as a living will or advanced directive
- Rigor mortis
Asystole is treated using the right branch of the Cardiac Arrest Algorithm. Click below to view the Cardiac Arrest Algorithm diagram. When done click again to close the diagram.
Cardiac Arrest Diagram
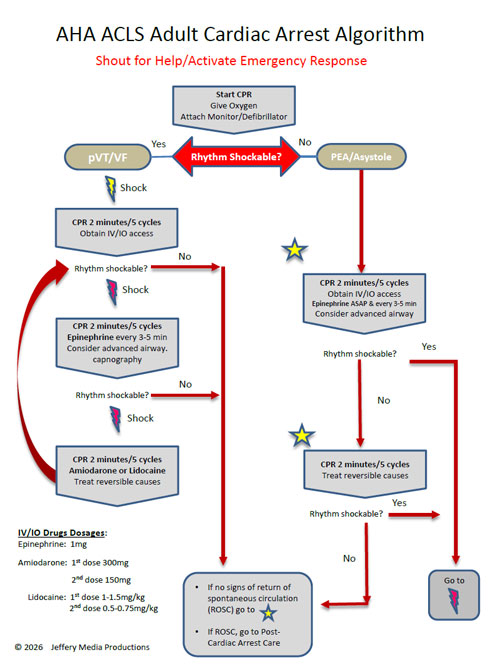
Members Download the Hi-Resolution PDF Here.
Vasopressors
A vasopressor is a medication that produces vasoconstriction and a rise in blood pressure. The vasopressor that is used for the treatment within the right branch of the Cardiac Arrest Algorithm is epinephrine.
Epinephrine is primarily used for its vasoconstrictive effects. Vasoconstriction is important during CPR because it will help increase blood flow to the brain and heart.
When treating asystole, epinephrine can be given as soon as possible but its administration should not delay initiation or continuation of CPR. After the initial dose, epinephrine is given every 3-5 minutes.
Rhythm checks should be performed after 2 minutes (5 cycles) of CPR. Limit rhythm checks to less than 10 seconds to minimize interruptions in CPR. Pulse checks should be performed when a rhythm check reveals a change in the rhythm to a rhythm that is organized and could be generating a pulse.