 Each ACLS algorithm is designed to simplify the process for the management and treatment of patients experiencing a cardiovascular emergency or progressing toward a cardiovascular emergency.
Each ACLS algorithm is designed to simplify the process for the management and treatment of patients experiencing a cardiovascular emergency or progressing toward a cardiovascular emergency.
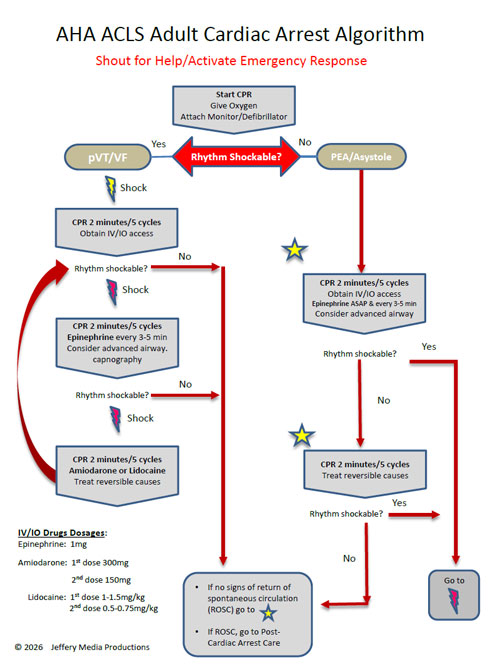
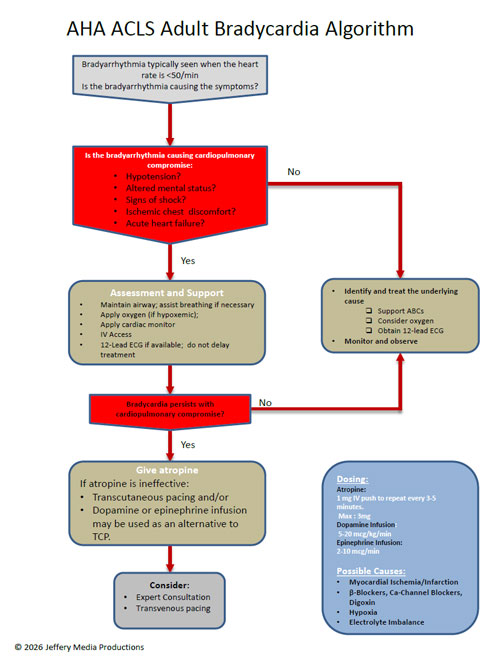
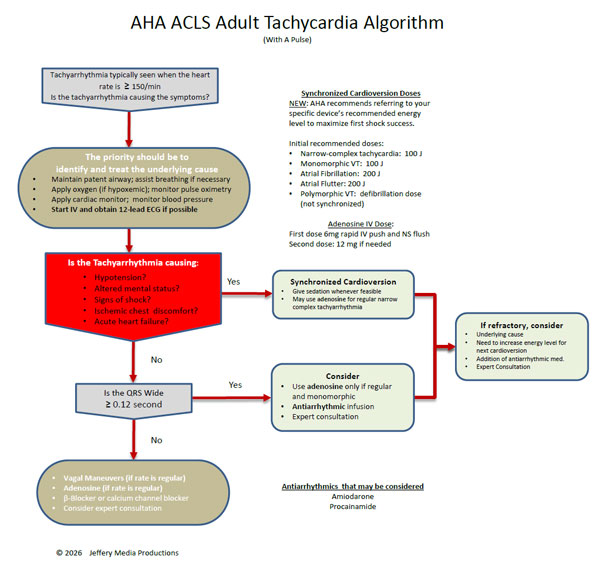
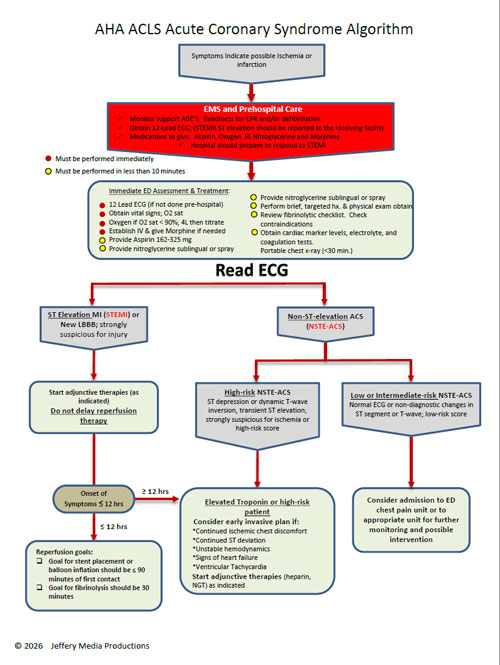
Most often these emergencies are related to an arrhythmia which must be identified and then treated with the appropriate ACLS algorithm.
Selection of the appropriate ACLS algorithm and path within the algorithm is determined by the type of arrhythmia present and the severity of the patient’s condition. Typically, the severity is classified as stable or unstable and this dictates interventions.
This ACLS algorithm overview, along with all of the pages of this website take the AHA ACLS algorithms and make them easy to understand and apply.
Jasmine says
I have a question: if the tachycardia has a patient that has BP over 90 systolic but has chest pain and AMS, is that unstable or stable?
On algorithm, BP under 90 is not only criteria for unstable- thanks for clarifying.
ACLS says
Your decision would depend upon what kind of tachycardia is identified. In all likelihood, this would be treated using the acute coronary syndrome algorithm unless a specific tachyarrhythmia that can be treated is identified.
Kind regards, Jeff
David says
Why is it that you cannot tap on each individual drug under primary heading “ACLS drugs” and learn about each drug. You use to be able to do this. Now you can only tap on the highlighted ‘red’ drugs to study. The idea simplicity. Now I have to go to the algorithm search there bounce back and forth.
Should be able to tap each individual drug and study on the “ACLS Drug “ heading.
David ICU/Cardiovascular Critical Care RN
WONDERFUL web site
Long time member and advocate to all new RN’s to purchase this web site!
ACLS says
Hi David,
my apologies there for the difficulties with the navigation.
This page is meant to be an overview and if you utilize the interactive course guide I think you will find that it is a much better way to navigate through all of the content.
Kind regards, Jeff
Ryan Allen says
boo hoo. click the buttons.
Jenny says
I feel like this is a dumb question but in an out patien procedure suit. MD, NP,RN only if a patient is severely bradycardic and atropine is not working and we dont have pacing available could we start an epi gtt with no pump? Is that appropriate?
ACLS says
An epinephrine drip in that situation would not be appropriate. You would want to treat the patient with BLS and call EMS. I would even hesitate to give atropine in that situation if you do not have the capability to further treat the patient if they continue to decline
Kind regards, Jeff
ryan says
That’s a scary proposition. first an outpatient procedural unit should have an automated defibrillator at least and if you are giving sedation at a facility like that then you should have a full defibrillator that has pacing and cardioversion capabilities. YOU REALLY SHOULD PACE THAT PATIENT. If you didn’t have that for some reason then an epi or dopamine drip could be considered but i would never run it without a pump. Running that with drip chamber titrations would be a nightmare, you may see hypertension, tackicardia or more ectopy or rhythm changes if you infuse too fast. Also your atropine push will only give you a transient bump in heart rate. Your patient may become bradycardic again in a few minutes. Getting ems rolling to you may be advisable.
Miranda Roberts Gosa says
I used this site as a student in my Respiratory Care program a couple years ago and flew through ACLS and PALS. I just reviewed the BLS scenarios prior to renewal and they are awesome as well. I’m going to purchase both ACLS and PALS for my renewal. Thank you for offering this program! Is there anyway you all could incorporate NRP simulations and practice?
ACLS says
Hi Miranda,
welcome back! I’m so glad that the site has been helpful for you. At the current time I do not have short term plans for adding NRP. If I get enough customers requesting NRP then that may become something that I work on in the future.
Kind regards, Jeff
Nadia says
I just finished taking the ACLS course at my hospital but am still unsure as to the frequency and timing of when to do a pulse check. I know that right after a shock, we must immediately proceed with compressions versus checking for a pulse, but can you advice as to when in the algorithm and how often we should be checking for a pulse and hence pause with compressions?
ACLS says
You will perform a pulse check after five cycles of CPR. The pulse check is performed with the rhythm check or after the rhythm check. Many people perform the pulse check with the rhythm check. This is the fastest way, but just realize that if the rhythm has not changed and a person remains in ventricular fibrillation then a pulse check is not necessary. You will first evaluate the rhythm quickly and then perform the pulse check.
When there are enough team members available it is prudent to check both at the same time. It makes the whole process just a little bit quicker.
Kind regards,
Jeff
Dr L M Yaqoob says
Thnx for providing such a golden tip
Ramesh Veeragandham says
I am a physician and do not participate in regular codes. Have to renew my ACLS. Site is very helpful and terrific. Great job and Thank you.
Ramesh
ACLS says
Thank you for the feedback. I’m so glad that the site has been helpful for you.
Kind regards, Jeff
Marcia Heng says
I have been using this site for several years and I must say, this page is a great addition! How you briefly describe the algorithms we use, color code them, and have links referencing each one. Brilliant for learning and putting it all together. Thank you for all you do!
ACLS says
Hi Marcia,
Thanks for the feedback!
Kind regards,
Jeff
Maria Cancel says
hello, is there a way that I can click on the algorithm and print it out? I think I was able to do it last time. I am a visual learner and printing the pictures will help me..
Jeff with admin. says
You can print out the algorithms by accessing the PDF files from the download library found here: Download Library
Kind regards,
Jeff
joemart1 says
Drop-down algorithms, videos, and practice tests are SO helpful? Just so well-organized, updated, and useful. Thanks again.