 Integrated post-cardiac arrest care is the 5th link in the AHA adult chain of survival. Topics of focus for post-cardiac arrest care include temperature control, hemodynamic and ventilation optimization, immediate coronary reperfusion with PCI (percutaneous coronary intervention), glycemic control, neurologic care and other technical interventions. To be successful, post-cardiac arrest care requires an integrated multidisciplinary approach.
Integrated post-cardiac arrest care is the 5th link in the AHA adult chain of survival. Topics of focus for post-cardiac arrest care include temperature control, hemodynamic and ventilation optimization, immediate coronary reperfusion with PCI (percutaneous coronary intervention), glycemic control, neurologic care and other technical interventions. To be successful, post-cardiac arrest care requires an integrated multidisciplinary approach.
For the purposes of this site, the review of post-cardiac arrest care interventions will focus primarily on immediate post-arrest interventions and aspects that you will most likely be tested on.
For a complete review of the subject refer to your AHA provider manual. (pages: 150-158)
Temperature Control
Temperature control which was previously called TTM (targeted temperature management) is the only intervention that has been shown to improve neurological outcomes after cardiac arrest. Temperature control should occur soon after ROSC (return of spontaneous circulation) for all cardiac arrest patients, and should be maintained for 36 hours. The decision point for the use of temperature control is whether or not the patient can follow commands. (lack of meaningful response to verbal commands)
Temperature control includes choosing one temperature between 32-37.5 °C (89.6-97.5 °F) and then holding that temperature for at least 36 hours. Common methods used for maintaining temperature control are endovascular catheter, surface cooling devices, or other simple surface cooling interventions.
During induced temperature control, the patient’s core temperature should be monitored with any one of the following: esophageal thermometer, a bladder catheter in the nonanuric patients, or a pulmonary artery catheter if one is already in place.
Axillary and oral temperatures are inadequate for monitoring core temperatures.
Ventilation Optimization
During the post-cardiac arrest phase, inspired oxygen should be titrated to maintain an arterial oxygen saturation of ≥90-98%. The goal is to avoid hypoxia and hyperoxia. This reduces the risk of oxygen toxicity. Excessive ventilation should also be avoided because of the potential for reduced cerebral blood flow related to a decrease in PaCO2 levels. Also, excessive ventilation should be avoided because of the risk of high intrathoracic pressures which can lead to adverse hemodynamic effects during the post-arrest phase.
Quantitative waveform capnography can be used to regulate and titrate ventilation rates during the post-arrest phase. Visit the link for more details about waveform capnography.
Avoid excessive ventilation. Ventilation should start at 10/min and should be titrated according to the target PETCO2 of 35-45 mmHg.
Hemodynamic Optimization
Hypotension, a systolic blood pressure < 90 mmHg should be treated and the administration of fluids and vasoactive medications can be used to optimize the patient’s hemodynamic status. While the optimal blood pressure during the post-cardiac arrest phase is not known, the primary objective is adequate systemic perfusion, and a mean arterial pressure of ≥ 65 mmHg should accomplish this. A mean arterial pressure ≥ 65 mmHg should be maintained during the post-cardiac arrest phase.
The goal of post-cardiac arrest care should be to return the patient to a level of functioning equivalent to their prearrest condition.
IV infusions for the control of post-arrest hypotension:
- IV Fluid Bolus: Give 1-2 L of normal saline or LR
- Epinephrine 2-10 mcg/min
- Dopamine 5-20 mcg/kg/min
- Norepinephrine 0.1-0.5 mcg/kg/min
Other considerations
Moderate glycemic control measures should be implemented to maintain glucose levels within a normal range, and since there is an increased risk for hypoglycemia, attention should be focused on prevention. No specific glycemic target range is recommended at this time.
Every effort should be made to provide coronary reperfusion (PCI), and interventions should be directed with this goal in mind. PCI has been shown to be safe and effective in both the alert and comatose patient, and hypothermia does not contraindicate PCI.
Click below to view the Post-Cardiac Arrest Algorithm Diagram. When finished, click again to close the diagram.
Post-Cardiac Arrest diagram
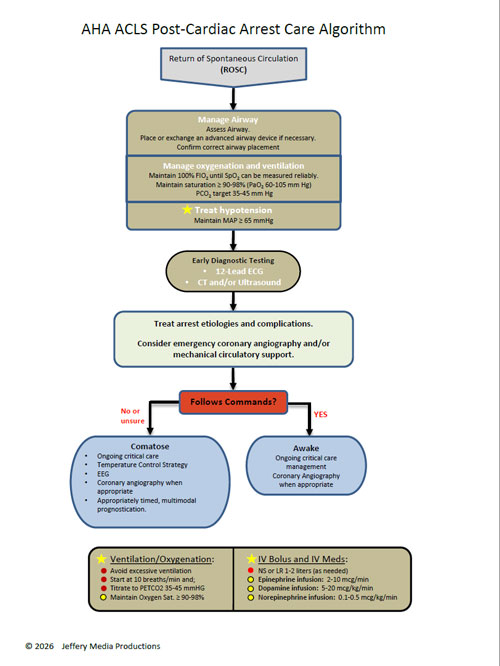
or Download the High Resolution PDF Here. (This will open in another window.)
malina bunbury says
Hi Jeff,
Today was my ACLS exams and I passed . I would like to take this opportunity to thank you for this great site . I will be advertising the site to my colleges . Once again thank you.
Malina.
Jeff with admin. says
Great job. I’m so glad that the site has been helpful for you. Kind regards,
Jeff
jeremin says
if the patient is in ROSC, has spontaneous breathing but unresponsive do we still need to intubate the patient? please sir jeff respond asap.
Jeff with admin. says
If the patient has spontaneous breathing and is maintaining adequate oxygenation per either a blood gas and pulse oximetry or Waveform Capnography then you would not have to intubate the patient. If the patient has spontaneous breathing but is not maintaining adequate oxygenation then you would intubate. Adequate oxygenation would be the deciding factor.
Kind regards,
Jeff
manalram says
Hi jeff, thanks for the other response. another question, i noticed you dont have the acute coronary syndrome algorithm on this site 🙁 maybe im not seeing it….
thank you!
Jeff with admin. says
Acute coronary syndrome is covered in the practice quizzes and also in the video department under ACLS algorithm videos.
Kind regards,
Jeff
jasonboivie says
Is an Amio maintenance infusion still recommended in ROSC if Amio was used in the cardiac arrest?
Thanks!
Jeff with admin. says
An Amiodarone infusion is only recommended if the patient has persistent arrhythmias in the post arrest phase that would indicate the use of amiodarone. Amiodarone is no longer recommended for prophylactic use just because it was used in the code and the patient seemed to respond. There is no evidence to show that using prophylactic amiodarone improves patient survival to hospital discharge.
Kind regards,
Jeff
T.J. says
Not to beat this dead horse into the ground but if I could pick your brain on a topic, it would greatly help in my instruction to students, as I seem to be butting heads with my supervisor.
As per ACLS (AHA) once a patient returns to spontanious circulation (ROSC), would you want to even consider TCP (pacing) an unresponsive patient if that patient is perfusing well either before or after providing the correct epi and dopamine ? My take on this is that as long as perfusion is above 90 systolic and O2 sats are being maintained above 94% (without hyperventilation) I don’t care that thes presenting with a Bradycardia rhythm… I see no need to pace the patient. Teaching students to pace an unstable/unreposive patient because heart rate is slow (in ROSC) is definately going to cause problems as the medication doseages used in an unstable bradycardia are different than that of ROSC. I have spoken to AHA District manager on this and he confirms that AHA will not take a stance on this and as such, pacing is not included in the flow diagram for treatment of ROSC. Your take on this ???
Jeff with admin. says
There would be no indication to pace the patient after ROSC unless the patient has persistent unstable bradycardia and the unstable condition has been determined to be related to the bradyarrhythmia. If the unstable condition is not related to a arrhythmia, you would use AHA (ROSC) post-arrest protocol to stabilize the patient.
Kind regards,
Jeff
adolson says
Under Hemodynamic Optimization there is a typo in the red oulined box – “the their”, Enjoying the online reading and I am finding it very helpful. I am a psych nurse with no hospital experience who just landed a new job in the ED. I need to know this information!!! Do you have any words of wisdom?
Jeff with admin. says
I’m so glad that the site has been helpful for you. I would encourage you to use the Interactive Course Guide to go through everything on the site. It will help guide you in your study. You can access the Interactive course guide from the home page and also from the top navigation. Please let me know if you have any questions. If you cover everything on the site, you will be thoroughly prepared for ACLS certification and also for code situations.
Also, Thanks for the spelling correction. I have corrected the error.
Kind regards,
Jeff
Kenneth Lübcke says
Hi.
I have a Question about cardiac arrest after the patient get ROSC?
Of the patient get ROSC after 3 shock, and 300mg amiodarone, at after little time get cardiac arrest again, what will the recommendation be! Will we start a New session whit 300mg after 3 shocks again or will we be in the first algorithm and give 150mg amiodarone after 2 shock (5shock)?
Jeff with admin. says
In a real scenario, you would give the dose of 150mg as soon as possible and then begin the maintenance infusion after the 150mg bolus.
If you are presented with this type of scenario during your certification ask for clarification if the instructor wants you to start at the beginning of the algorithm or where you left off after the first ROSC.
Hope that makes sense.
Kind regards,
Jeff
Terrystill1 says
This is such a great site Jeff. I am so glad I found it and I will definitely recommend it to my co-workers . Thank you
Jeff with admin. says
Thanks for the feedback and thank you for recommending the site!
Kind regards,
Jeff
David says
So in my ACLS class we came upon the question of when you achieve ROSC and the heart rate is bradycardic, why don’t you go into the bradycardia algorithm instead of the ROSC algorithm. From what I thought it was the timing of it and that you should use the ROSC algorithm because you actually did just get there. But in the ROSC algorithm there is no medication choice for atropine and also wouldn’t therapudic hypothermia make the heart slower eventually?
It it one algorithm or another or are you supposed to combine them both?
Jeff with admin. says
This can sometimes be a little tricky because it is likely in the ROSC as the heart recovers, the patient may experience bradycardia. There are actually medications that can and are used in the ROSC Post arrest phase. They are medication infusions used to treat hypotension. Fortunately, two of these medications are the same medications used for chemical pacing in the bradycardia algorithm. Epinephrine and dopamine.
So if the patient has symptomatic bradycardia after ROSC you are going to see hypotension. Use epinephrine or dopamine for hypotension and you will most likely see the patient hypotension correct and the HR will also improve.
Hope that makes sense.
Kind regards,
Jeff
ivette bermeo says
When is hypothermia contraindicated. Thanks.
Jeff with admin. says
“There are few true contraindications for TH. Medical conditions in which the risk may be excessive include documented intracranial hemorrhage, severe hemorrhage leading to exsanguination, hypotension refractory to multiple vasopressors, severe sepsis, and pregnancy. Given that most patients from CA die of neurological consequences for which TH is the only proven beneficial therapy, the decision to withhold TH must be weighed carefully.”
AHA reference for Quote.
Kind regards,
Jeff
Ryan says
therapeutic hypothermia is contraindicated when pt is under 16 y/o or has meaningful response (alert and oriented).
ashrafudheen says
its good to learn thanks alot
JOJO says
Thank you for this website, recertifying since last cert was 4 years ago. Very helpful.
Edward says
There is a well powered study published in NEJM 2013;369: 2197-2206 pointing at no benefit for target temperatures of 33 celsius in out-of-hospital cardiac arrest patients. The 2014 ACLS guidelines still advice 32-34 celsius in postcardiac arrest care. Is there a preliminary ACLS position on this especific subject?
Jeff with admin. says
I have not seen any direct statements from AHA. This information has been presented and I’m sure that we will see something by the end of 2015. The following article covers the topic well: Therapeutic Hypothermia.
Kind regards,
Jeff
MICHAEL GUTH says
There is no evidence to support continued prophylactic administration of antiarrhythmic medications once the patient achieves ROSC. page 77. This is actually on one of the practice exams of the ACLS student site. I find the statement confusing, I take it that it does not mean that an amniodarone infusion should be terminated….
Jeff with admin. says
It means that you would not need to start a post-cardiac arrest infusion just because amiodarone was used during the cardiac arrest. You would only start an amiodarone infusion if any tachyarrhythmias persist in the post-arrest period.
Kind regards,
Jeff
tomoms says
Incredible course and so easy to navigate. Also very thorough. Having been an ACLS instructor back in the early 80’s with no technology like this to help study, I find this incredible. I am a surgeon and have to re-certify every 2 years so this is great. Thanks Jeff.