 Integrated post-cardiac arrest care is the 5th link in the AHA adult chain of survival. Topics of focus for post-cardiac arrest care include temperature control, hemodynamic and ventilation optimization, immediate coronary reperfusion with PCI (percutaneous coronary intervention), glycemic control, neurologic care and other technical interventions. To be successful, post-cardiac arrest care requires an integrated multidisciplinary approach.
Integrated post-cardiac arrest care is the 5th link in the AHA adult chain of survival. Topics of focus for post-cardiac arrest care include temperature control, hemodynamic and ventilation optimization, immediate coronary reperfusion with PCI (percutaneous coronary intervention), glycemic control, neurologic care and other technical interventions. To be successful, post-cardiac arrest care requires an integrated multidisciplinary approach.
For the purposes of this site, the review of post-cardiac arrest care interventions will focus primarily on immediate post-arrest interventions and aspects that you will most likely be tested on.
For a complete review of the subject refer to your AHA provider manual. (pages: 150-158)
Temperature Control
Temperature control which was previously called TTM (targeted temperature management) is the only intervention that has been shown to improve neurological outcomes after cardiac arrest. Temperature control should occur soon after ROSC (return of spontaneous circulation) for all cardiac arrest patients, and should be maintained for 36 hours. The decision point for the use of temperature control is whether or not the patient can follow commands. (lack of meaningful response to verbal commands)
Temperature control includes choosing one temperature between 32-37.5 °C (89.6-97.5 °F) and then holding that temperature for at least 36 hours. Common methods used for maintaining temperature control are endovascular catheter, surface cooling devices, or other simple surface cooling interventions.
During induced temperature control, the patient’s core temperature should be monitored with any one of the following: esophageal thermometer, a bladder catheter in the nonanuric patients, or a pulmonary artery catheter if one is already in place.
Axillary and oral temperatures are inadequate for monitoring core temperatures.
Ventilation Optimization
During the post-cardiac arrest phase, inspired oxygen should be titrated to maintain an arterial oxygen saturation of ≥90-98%. The goal is to avoid hypoxia and hyperoxia. This reduces the risk of oxygen toxicity. Excessive ventilation should also be avoided because of the potential for reduced cerebral blood flow related to a decrease in PaCO2 levels. Also, excessive ventilation should be avoided because of the risk of high intrathoracic pressures which can lead to adverse hemodynamic effects during the post-arrest phase.
Quantitative waveform capnography can be used to regulate and titrate ventilation rates during the post-arrest phase. Visit the link for more details about waveform capnography.
Avoid excessive ventilation. Ventilation should start at 10/min and should be titrated according to the target PETCO2 of 35-45 mmHg.
Hemodynamic Optimization
Hypotension, a systolic blood pressure < 90 mmHg should be treated and the administration of fluids and vasoactive medications can be used to optimize the patient’s hemodynamic status. While the optimal blood pressure during the post-cardiac arrest phase is not known, the primary objective is adequate systemic perfusion, and a mean arterial pressure of ≥ 65 mmHg should accomplish this. A mean arterial pressure ≥ 65 mmHg should be maintained during the post-cardiac arrest phase.
The goal of post-cardiac arrest care should be to return the patient to a level of functioning equivalent to their prearrest condition.
IV infusions for the control of post-arrest hypotension:
- IV Fluid Bolus: Give 1-2 L of normal saline or LR
- Epinephrine 2-10 mcg/min
- Dopamine 5-20 mcg/kg/min
- Norepinephrine 0.1-0.5 mcg/kg/min
Other considerations
Moderate glycemic control measures should be implemented to maintain glucose levels within a normal range, and since there is an increased risk for hypoglycemia, attention should be focused on prevention. No specific glycemic target range is recommended at this time.
Every effort should be made to provide coronary reperfusion (PCI), and interventions should be directed with this goal in mind. PCI has been shown to be safe and effective in both the alert and comatose patient, and hypothermia does not contraindicate PCI.
Click below to view the Post-Cardiac Arrest Algorithm Diagram. When finished, click again to close the diagram.
Post-Cardiac Arrest diagram
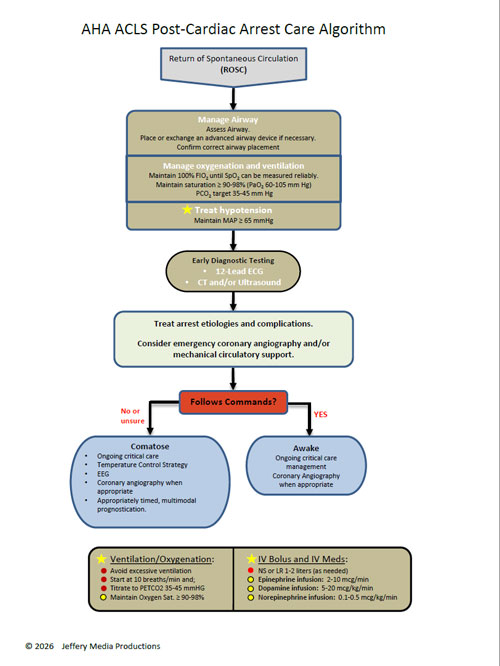
or Download the High Resolution PDF Here. (This will open in another window.)
Neville says
This course work was surprisingly eye-opening and thorough. ACLS has changed much through the years. Thank you.
shafi says
i found it very good
Rosamachado says
I agree great site second time using and have recommended it to my friends and coworkers, thank you you Jeff!
Jeff with admin. says
I’m glad that the site has been helpful for you.
Kind regards,
Jeff
kathleenflynn says
LOVE THIS SITE WORTH EVERY PENNY GREAT PRACTICE WITH WELL PRESENTED SCENARIOS THNX
Joe says
A good easy way to remember ROSC that I was taught is B.L.E.A.C.H.O.
Blood Pressure = >90 mmHg
Labs = Draw
EKG = Obtain 12-Lead
Advanced Airway = ETT, Supraglottic
Capnography = 35-40 mmHg During Arrest = >10 mmHg
Hypothermia = Ice Packs, Cold Fluids Maintain 32-34 Celsius
Oxygen = Maintain SpO2 >94%
This is what my teacher taught and it helped me remember very easily!!!! Hope it helps!!!
Jeff with admin. says
I like that thank you for sharing. Kind regards, Jeff
Rick Raub says
In response to the previous question: We always Temp correct ABG’s during code cool. When a pt is cold (32-34), the actual P02 is lower than what a non temp corrected ABG shows. It may look like an acceptable value result but when you temp correct it can sometimes drop into the critical value category, and often does. Plus the C02 shows a false lower value with non-temp corrected ABG.
Thanks for this great resource. Im taking the ACLS class soon and am soaking up my brain with all this info ahead of time.
sofia says
Jeff;;What medical scenarios can I expect in a Interview for the Cruise Ships/
Jeff with admin. says
You will probably be have to show proficiency with BLS and ACLS and have a basic working knowledge of cardiac care, trauma, and internal medicine.
Kind regards,
Jeff
Matt Weed says
Hello Sir,
My name is Matt and I just got done running a Code with my crew. Minimal downtime-maybe 1 min of good bystander CPR prior to our arrival-pt in v-fib-shocked once- went into a narrow complex tachycardia @130. I gave Lidocaine 1.5mg/kg and started packaging the patient.
While packaging, the pt lost pulses and went into v-fib again so we shocked him again. Again he went into a perfusing rhythm, which he stayed in for the rest of our call.
My question, are we not to do this anymore? One of my newer/younger co-workers asked me after the call “I don’t think we do that anymore?”, i.e. giving Lidocaine post conversion. It was very cute he didn’t want to go against the ‘ol veteran medic…
I’ve been a medic since 1998 and have gone through numerous ACLS recertifications. In fact I just renewed my ACLS cert and apparently got through the process without hearing this. My young partner states we just go to the rosc algorithm without Lido..?
Jeff with admin. says
There is no evidence that the prophylactic use of amiodarone or lidocaine in the post-arrest phase changes mortality rates or increased survival to hospital discharge. However, if a patient is shocked and then converts to a perfusing rhythm and then has more arrhythmia, amiodarone or lidocaine would be indicated.
Simplified:
If you shock VF/pulseless VT once and the patient coverts. If they do not experience any other arrhythmias then there would be no need to prophylacticly start a lidocaine or amiodarone infusion.
If you shock VF/pulseless VT, the patient converts, then has arrhythmias or has recurrent VF/pulseless VT, then amiodarone or lidocaine would be indicated for the prevention of further arrhythmias.
I hope this makes sense.
Great job on the resuscitation by the way!
Kind regards,
Jeff
Lauren Hunt says
What is the recommendation as to the time frame for implementing therapeutic hypothermia post cardiac arrest? For instance, how long is too long too wait?
Jeff with admin. says
Therapeutic hypothermia should be initiated as soon as possible in the post arrest phase.
Kind regards,
Jeff
Nicki says
Jeff, earlier you posted a link for your post cardiac care algorithm. I am unable to locate it. Would you post again, please? and include in your download library? Thank you much.
Jeff with admin. says
I will try and get a diagram put in the download library soon. Until then, you can find an image of the diagram here.
Mark Obenauer says
What is stability of IV fluid normal saline and lactate ringers stored in original wrapper refrigerated?
Jeff with admin. says
LR and NS are stable in their own containers when refrigerated.
Kind regards,
Jeff
Lindsay says
Hi there, I was just wondering if there is somewhere that I could find a list of labs that should/need to be drawn and how often when it comes to the protocol? I am familiar with initiating the protocol from years as a trauma nurse but most recently am working in a hospital that does not use the protocol very often (because lack of necessity). I am trying to create an easy to follow tip sheet to assist staff with initating and maintaining the hypothermia. Does the AHA have recommendations for lab work?
Thank you,
Lindsay
Chris with admin. says
The AHA does not have a specific protocol for labs to be drawn post-arrest. The labs and diagnostic tests that should be performed should center around management of post-cardiac arrest syndrome. I do not have a specific protocol but the article in the link below will help you in easily developing one.
Kind Regards,
Chris
Management of Post-Arrest
chrisflan says
I am an Australian Anaesthetic Nurse, and we too use Meperidine (AKA Pethidine) for post shivering. I have discussed this with Anaesthetists in the past, and they say this is the first choice drug for shivering (although there is little research/evidence available to verify this, it seems to be more anecdotal evidence). Cheers.
Terry Lyster says
Hi Jeff,
Quick question for you. One of my ACLS students stated she was in a code recently in the emergency room and was the med nurse. She gave the IVP EPI per order and was getting ready to follow it with a 20cc bolus (as she was taught per AHA guidleine) when the ER nurses stopped her and said “we don’t do that down here since we have our saline running “wide open”. The IV was a peripheral site. What are your thoughts on this? I only could find the AHA’s recommendation on the flush and elevating the extremity. Is having an IV wide open considered enough to get that EPI to the central circulatory system?
Terry
Jeff with admin. says
I would follow the AHA recommendations. If you have fluids running, flush the 20mls of NS right in after it and leave the fluids running. This will bolus the epinephrine into the circulatory system much more effectively than just the IV Fluids running on a pump.
Kind regards,
Jeff
Lovely says
When optimizing blood pressure, can you mix PNSS with Dopa (2-10 mcg/kg/min) to be infused, or do you administer the IV fluids (PNSS or LR) first, then Dopamine infusion next, if IV fluids didn’t work out?
Jeff with admin. says
In the post arrest phase, the dopamine infusion should be a separate single infusion. Any fluid resuscitation should be given separately. You can run IVF of NS or LR in a separate single line and can run the dopamine in another separate line. These can be Y-ported together but the infusions should be run separately but they can be infused simultaneously.
Kind regards,
Jeff