 Integrated post-cardiac arrest care is the 5th link in the AHA adult chain of survival. Topics of focus for post-cardiac arrest care include temperature control, hemodynamic and ventilation optimization, immediate coronary reperfusion with PCI (percutaneous coronary intervention), glycemic control, neurologic care and other technical interventions. To be successful, post-cardiac arrest care requires an integrated multidisciplinary approach.
Integrated post-cardiac arrest care is the 5th link in the AHA adult chain of survival. Topics of focus for post-cardiac arrest care include temperature control, hemodynamic and ventilation optimization, immediate coronary reperfusion with PCI (percutaneous coronary intervention), glycemic control, neurologic care and other technical interventions. To be successful, post-cardiac arrest care requires an integrated multidisciplinary approach.
For the purposes of this site, the review of post-cardiac arrest care interventions will focus primarily on immediate post-arrest interventions and aspects that you will most likely be tested on.
For a complete review of the subject refer to your AHA provider manual. (pages: 150-158)
Temperature Control
Temperature control which was previously called TTM (targeted temperature management) is the only intervention that has been shown to improve neurological outcomes after cardiac arrest. Temperature control should occur soon after ROSC (return of spontaneous circulation) for all cardiac arrest patients, and should be maintained for 36 hours. The decision point for the use of temperature control is whether or not the patient can follow commands. (lack of meaningful response to verbal commands)
Temperature control includes choosing one temperature between 32-37.5 °C (89.6-97.5 °F) and then holding that temperature for at least 36 hours. Common methods used for maintaining temperature control are endovascular catheter, surface cooling devices, or other simple surface cooling interventions.
During induced temperature control, the patient’s core temperature should be monitored with any one of the following: esophageal thermometer, a bladder catheter in the nonanuric patients, or a pulmonary artery catheter if one is already in place.
Axillary and oral temperatures are inadequate for monitoring core temperatures.
Ventilation Optimization
During the post-cardiac arrest phase, inspired oxygen should be titrated to maintain an arterial oxygen saturation of ≥90-98%. The goal is to avoid hypoxia and hyperoxia. This reduces the risk of oxygen toxicity. Excessive ventilation should also be avoided because of the potential for reduced cerebral blood flow related to a decrease in PaCO2 levels. Also, excessive ventilation should be avoided because of the risk of high intrathoracic pressures which can lead to adverse hemodynamic effects during the post-arrest phase.
Quantitative waveform capnography can be used to regulate and titrate ventilation rates during the post-arrest phase. Visit the link for more details about waveform capnography.
Avoid excessive ventilation. Ventilation should start at 10/min and should be titrated according to the target PETCO2 of 35-45 mmHg.
Hemodynamic Optimization
Hypotension, a systolic blood pressure < 90 mmHg should be treated and the administration of fluids and vasoactive medications can be used to optimize the patient’s hemodynamic status. While the optimal blood pressure during the post-cardiac arrest phase is not known, the primary objective is adequate systemic perfusion, and a mean arterial pressure of ≥ 65 mmHg should accomplish this. A mean arterial pressure ≥ 65 mmHg should be maintained during the post-cardiac arrest phase.
The goal of post-cardiac arrest care should be to return the patient to a level of functioning equivalent to their prearrest condition.
IV infusions for the control of post-arrest hypotension:
- IV Fluid Bolus: Give 1-2 L of normal saline or LR
- Epinephrine 2-10 mcg/min
- Dopamine 5-20 mcg/kg/min
- Norepinephrine 0.1-0.5 mcg/kg/min
Other considerations
Moderate glycemic control measures should be implemented to maintain glucose levels within a normal range, and since there is an increased risk for hypoglycemia, attention should be focused on prevention. No specific glycemic target range is recommended at this time.
Every effort should be made to provide coronary reperfusion (PCI), and interventions should be directed with this goal in mind. PCI has been shown to be safe and effective in both the alert and comatose patient, and hypothermia does not contraindicate PCI.
Click below to view the Post-Cardiac Arrest Algorithm Diagram. When finished, click again to close the diagram.
Post-Cardiac Arrest diagram
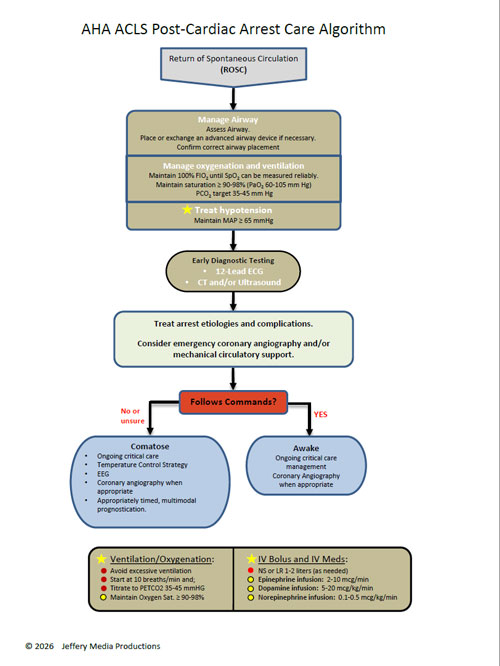
or Download the High Resolution PDF Here. (This will open in another window.)
Robert Kuklok says
How fast of an infusion of cold iv solution and can this cause fluid overload or work on the heart?
Jeff with admin. says
This would be completely dependent upon the situation. Caution should always be used when giving any type of fluid during the post arrest phase.
The infusion of cooled saline solution is targeted to a volume of 30 ml/kg and a maximum rate of 100 ml/min to achieve the targeted temperature.
Kind regards,
Jeff
Teresa DiLena says
Thank you Jeff for your quick response.
Jeff with admin. says
You are welcome! Kind regards, Jeff
GregW says
Regarding MAP. I find that using a different calculation for MAP is easier to do without paper and pencil (or calculator): ((Systolic-Diastolic)/3) + D. This is: adding 1/3 of the difference between the systolic and diastolic pressures to the diastolic.
Anne says
Love this! Thank you.
Flow Simmons says
Thank you for keeping your explanations very simple.
Jeff with admin. says
Glad to help! Kind regards, Jeff
Light says
Hypothermia I believed is no longer advised .
Jeff with admin. says
It is now called TTM (targeted temperature management). It is managed slightly different since the new 2015 guideline changes. Kind regards, Jeff
Dr Syed Ashraf says
I really appreciate the way you simplify things and make it clear
Thank you very much
Dr Syed Ashraf says
Hi sir
your opinion regarding Moderate glycemic control measures should be implemented to maintain glucose levels from 144-180 mg/dL is questioned by one of our ACLS instructor as it is not mentioned in ACLS manual. kindly let me know the reference
Jeff with admin. says
Your instructor is correct. This change was overlooked when we updated to the latest AHA ACLS guidelines. Thank you for pointing this out. I have updated the information for correction.
Here is the AHA position:
“Healthcare providers should not attempt to alter glucose concentration within a lower range (80-100 mg/dL), because of the increased risk of hypoglycemia. The 2015 AHA guidelines update for CPR and ECC does not recommend any specific target range of glucose management in adults with ROSC after cardiac arrest.”
My apologies for the confusion on the post-cardiac arrest glycemic control measures.
Kind regards,
Jeff
Ray Taylor says
In a scenario of post-cardiac arrest, EKG: irregular tachycardia (HR >150) with an unstable BP, should i follow the “unstable tachycardia algorithm” or is there any other special consideration i should keep in mind?
Thank you in advance
Jeff with admin. says
You would follow the unstable tachycardia algorithm.
As with any cardiac emergency, you would need to consider any underlying causes and seek expert consultation as soon as possible.
Kind regards,
Jeff
Rachel Jolokai says
Hey Jeff,
What is the difference between BP and mean arterial pressure? How do you calculate it and when is one more helpful than the other?
Jeff with admin. says
“MAP, or mean arterial pressure, is defined as the average pressure in a patient’s arteries during one cardiac cycle. It is considered a better indicator of perfusion to vital organs than systolic blood pressure (SBP). A true MAP can only be determined by invasive monitoring and complex calculations; however, it can also be calculated using a formula of the SBP and the diastolic blood pressure (DBP).”
The simple way to estimate the patient’s MAP is to use the following formula: MAP = [ (2 x diastolic) + systolic ] divided by 3. The reason that the diastolic value is multiplied by 2, is that the diastolic portion of the cardiac cycle is twice as long as the systolic.
Ref:
1-Calculating MAP
2-Calculating MAP
Kind regards,
Jeff
Anne O Brien says
This is brilliant, I get it now, thank you.
Ranjini Pushparaja says
Is there a particular time frame in terms of definition for ROSC?
Jeff with admin. says
there is no particular time frame in terms of the definition for ROSC.
There are many variables that can affect ROSC. Time is an important factor and a resuscitation team must take this into consideration.
Probably the most important factor that will affect ROSC and your continuation of CPR will be an adequate end tidal CO2.
ETCO2 will give you a good gauge of whether your patient can achieve ROSC.
Kind regards,
Jeff
Tehetena Zarou says
Hi Jeff,
Thanks so much for the valuable information and the excellent presentation.
A few questions;( hope not too many)
TTM; How is a single targeted temperature selected and maintained?
In terms of acheiving hemodynamic stability and maintaining normoglyacaemia ,how does it go hand in hand with TTM?
Also how best can ventilation be optimised in the abscence of wave capnography
Kind regards
Jeff with admin. says
Question 1:
One of the most common methods used for inducing therapeutic hypothermia is a rapid infusion of ice-cold (4° C), isotonic, non-glucose-containing fluid to a volume of 30 ml/kg. The optimum temperature for therapeutic hypothermia is 32-36 ° C (89.6 to 96.8 ° F). A single target temperature, within this range, should be selected, achieved, and maintained for at least 24 hours. This specific temperature selection within the range of 32-36 ° C, allows for tight control of the temperature.
Question 2:
Achieving hemodynamic stability, normoglycemia, and TTM all work together to preserve and reestablish normal neurologic function.
Question 3:
If there is no availability to monitor waveform capnography, good chest rise and fall and maintenance of an adequate airway are the two best methods for ensuring that adequate ventilation’s are being provided.
Kind regards,
Jeff
Foxju says
ACLS info/ updates and PALS sites are amazing!!
THANK YOU!
Wish you’d do ATLS too!
????
Mathismi says
hi Jeff so happy you are still here and that you have added PALS to your teaching
thank you so much
shelly
Jeff with admin. says
You are very welcome. Kind regards, Jeff
Prabin Kumar Jha says
Thank you for valuable informations. Great help for residents.
Jeff with admin. says
Excessive ventilation causes decreased PaCO2 which subsequently leads to arterial vasoconstriction thus lowering cerebral blood flow (CBF), and cerebral blood volume. This effect is mediated my pH changes in the extracellular fluid which cause cerebral vasoconstriction or vasodilation depending on the pH.