 Integrated post-cardiac arrest care is the 5th link in the AHA adult chain of survival. Topics of focus for post-cardiac arrest care include temperature control, hemodynamic and ventilation optimization, immediate coronary reperfusion with PCI (percutaneous coronary intervention), glycemic control, neurologic care and other technical interventions. To be successful, post-cardiac arrest care requires an integrated multidisciplinary approach.
Integrated post-cardiac arrest care is the 5th link in the AHA adult chain of survival. Topics of focus for post-cardiac arrest care include temperature control, hemodynamic and ventilation optimization, immediate coronary reperfusion with PCI (percutaneous coronary intervention), glycemic control, neurologic care and other technical interventions. To be successful, post-cardiac arrest care requires an integrated multidisciplinary approach.
For the purposes of this site, the review of post-cardiac arrest care interventions will focus primarily on immediate post-arrest interventions and aspects that you will most likely be tested on.
For a complete review of the subject refer to your AHA provider manual. (pages: 150-158)
Temperature Control
Temperature control which was previously called TTM (targeted temperature management) is the only intervention that has been shown to improve neurological outcomes after cardiac arrest. Temperature control should occur soon after ROSC (return of spontaneous circulation) for all cardiac arrest patients, and should be maintained for 36 hours. The decision point for the use of temperature control is whether or not the patient can follow commands. (lack of meaningful response to verbal commands)
Temperature control includes choosing one temperature between 32-37.5 °C (89.6-97.5 °F) and then holding that temperature for at least 36 hours. Common methods used for maintaining temperature control are endovascular catheter, surface cooling devices, or other simple surface cooling interventions.
During induced temperature control, the patient’s core temperature should be monitored with any one of the following: esophageal thermometer, a bladder catheter in the nonanuric patients, or a pulmonary artery catheter if one is already in place.
Axillary and oral temperatures are inadequate for monitoring core temperatures.
Ventilation Optimization
During the post-cardiac arrest phase, inspired oxygen should be titrated to maintain an arterial oxygen saturation of ≥90-98%. The goal is to avoid hypoxia and hyperoxia. This reduces the risk of oxygen toxicity. Excessive ventilation should also be avoided because of the potential for reduced cerebral blood flow related to a decrease in PaCO2 levels. Also, excessive ventilation should be avoided because of the risk of high intrathoracic pressures which can lead to adverse hemodynamic effects during the post-arrest phase.
Quantitative waveform capnography can be used to regulate and titrate ventilation rates during the post-arrest phase. Visit the link for more details about waveform capnography.
Avoid excessive ventilation. Ventilation should start at 10/min and should be titrated according to the target PETCO2 of 35-45 mmHg.
Hemodynamic Optimization
Hypotension, a systolic blood pressure < 90 mmHg should be treated and the administration of fluids and vasoactive medications can be used to optimize the patient’s hemodynamic status. While the optimal blood pressure during the post-cardiac arrest phase is not known, the primary objective is adequate systemic perfusion, and a mean arterial pressure of ≥ 65 mmHg should accomplish this. A mean arterial pressure ≥ 65 mmHg should be maintained during the post-cardiac arrest phase.
The goal of post-cardiac arrest care should be to return the patient to a level of functioning equivalent to their prearrest condition.
IV infusions for the control of post-arrest hypotension:
- IV Fluid Bolus: Give 1-2 L of normal saline or LR
- Epinephrine 2-10 mcg/min
- Dopamine 5-20 mcg/kg/min
- Norepinephrine 0.1-0.5 mcg/kg/min
Other considerations
Moderate glycemic control measures should be implemented to maintain glucose levels within a normal range, and since there is an increased risk for hypoglycemia, attention should be focused on prevention. No specific glycemic target range is recommended at this time.
Every effort should be made to provide coronary reperfusion (PCI), and interventions should be directed with this goal in mind. PCI has been shown to be safe and effective in both the alert and comatose patient, and hypothermia does not contraindicate PCI.
Click below to view the Post-Cardiac Arrest Algorithm Diagram. When finished, click again to close the diagram.
Post-Cardiac Arrest diagram
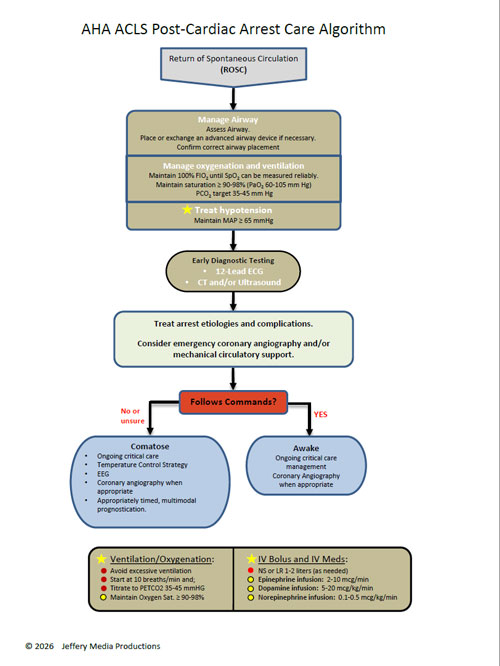
or Download the High Resolution PDF Here. (This will open in another window.)
Maryam says
Hello,
Pt at the ED with history of trauma (stap wound to chest – suspected haemothorax) passed into cardiac arrest
Pt intubated – started cpr- and the e.c.g monitor recorded shockable rhythm
Is it possible to start defibrillation without chest decompression nor restoring blood volume?
Thanks.
ACLS says
In the scenario, electrical defibrillation will do little to help the situation because the cause of the cardiac arrest has not been resolved or improved.
Electrical defibrillation would not be effective for the management of cardiac arrest due to trauma.
In cases of trauma-related cardiac arrest, addressing the underlying cause, such as controlling bleeding and providing other necessary interventions, takes precedence over defibrillation.
Kind regards,
Jeff
Mary says
Do you use defibrillator to manage traumatic cardiac shock ( severe haemorrhage).?
ACLS says
Defibrillation would not be used to manage traumatic, cardiac shock. He would treat the cause. You would need to stabilize the patient with fluid and blood and then manage other problems, such as ventricular, relation, bradycardia, or tachycardia.
Kind regards,
Jeff
Lori says
I work in an an ICU that is not currently doing TTM for post cardiac arrest patients. I’m not sure why we don’t but I’m trying to help. Can you point me to literature to help me share with the hospital why we need to start doing this? I know it preserves brain function, etc. Also one of our supervisors said that TTM would be contraindicated in a post cardiac arrest patient who was septic. Is this correct? I’ve never heard of a distinction like that so I wanted to check.
Thank you so much!
Lori
ACLS says
Thank you for the question about targeted temperature management. The link below is to the definitive reference from the circulation journal regarding targeted temperature management. There are reference links too much of the literature regarding this subject. I think you’ll find this the best reference. Circulation Journal Article
Kind regards,
Jeff
Ems says
Sir what is the rate of cold fluid when initiating TTM?Thanks
ACLS says
The American Heart Association does not provide specific details with regard to infusion rate for The administration of ice called isotonic fluids for targeted temperature management. In their literature it states “rapid iv infusion.”
This would implies that the infusion of fluid should be rapidly infused but slower than a bolus I would assume that the 1 L infusion would be administered in no more than one hour and preferably in under 15 minutes.
Kind regards,
Jeff
Ela Kowalski says
Can we use Sequential Compression Device (SCD) as an adjunct to pharmacological DVT prophylaxis while patient is undergoing TTM? Or should we rely only on Pharmacological DVT prophylaxis?
ACLS says
If you are referring strictly to DVT prophylaxis then SCD therapy would be just as efficient as pharmacological DVT prophylaxis. If you are including thrombus prevention related to prevention of MI then you need to rely on pharmacological prophylaxis.
Kind regards,
Jeff
gul sher afridi says
This is more than enough.
Allah bless u all.
Amanda says
Is there a time set for how long we should wait to make sure we truly have ROSC? Or is it we have capnogrophy and pulse and we automatically go to the post ROSC care algorithm right away.
ACLS says
If you are at the step of a rhythm/pulse check and you establish that the pulse is present then you will begin the post cardiac arrest care algorithm.
The same is true with regard to capnography. If you are providing CPR for 2 minutes and you see the ETCO2 rise to 35-45 mmHg then you would initiate the post-cardiac arrest care algorithm at the end of the 2 minute cycle of CPR.
Kind regards,
Jeff
Mustafa says
Hi Jeff
If patient developed cardiac arrest, it is important to give him IVF N.S running drop during resuscitation …
2. 2nd rescue arrived with AED , It is necessary to 1st rescu to complete 2 mit of cycle CPR and handover AED to 1st rescue or no need to complete 2 mit of CPR immediately handover AED to 1st resuc
ACLS says
1. Having a running IV fluid drip of NS Is convenient but not necessary. You just need to ensure that all medications are followed with a 20 mL rapid IV push of NS.
2. This depends upon the situation. If this was a witnessed arrest then once the AED arrives, CPR can be immediately stopped to attach the AED and analyze the rhythm.
If this was a unwitnessed arrest then once the AED arrives, the two minutes of CPR should be completed and then the AED attached in the rhythm and analyzed.
Kind regards,
Jeff
Tatiana Guerra gonzalez says
ES EXCELENTE EL CURSO GRACIAS
ACLS says
Thanks! ☺️
alexander vinckenbosch says
Also verry important is to Ensure your patiënt head would be in a 30° angle due to the fact that a elevation of the head could help to fight a increase in ICP.
an nguyen says
What are your thoughts on steroids post cardiac arrest?
Jeff with admin. says
I do not have a specific opinion about this subject as I do not have any experience with use of routine steroid administration during the post cardiac arrest phase.
I can refer you to a recently published article found in the link below.
The article seems to indicate that routine steroid use may slightly improve outcomes, but more research is needed.
Post-Cardiac Arrest Steroid Use
Kind regards,
Jeff
Kelli S. says
In the setting of Out of Hospital Cardiac Arrest (OHCA) is there a recommended time frame before initiating transport post ROSC? Is there a greater risk of re-arrest moving the patient too quickly?
Jeff with admin. says
Immediate transport to a higher level of care in post-arrest after ROSC is recommended. As far as I know, there is not an increased risk of rearrest during transport.
Early access to PCI is of great importance and this would demand rapid transport.
Overall, early access to a higher level of care for PCI and neurological intensive care is desired after ROSC. The earlier the post-arrest interventions are implemented the better the outcomes.
As a caveat, there is literature that indicates that CPR performed during transport may decrease ROSC due to poor quality of cpr performed. In other words, it appears that is is better to obtain ROSC and then transport.
Kind regards,
Jeff
Mark E Vanmaren says
Kelli (and Jeff),
EMS protocols in my region specify that after ROSC is obtained the pt should be observed but not moved for 10 minutes. During this time there is certainly plenty to do: obtain blood pressure, 12L EKG, any appropriate blood tests, consult with family, hang a vasopresser drip, arrange for a crew of responders to accompany in the rig in case of re-arrest, get the means of moving the pt in place (backboard, Megamover, etc).
We have found that if we move the pt too soon re-arrest goes undetected for a bit due to us having the patient in a stairwell,a side yard, or out in the rain, etc, where no one is able to closely monitor status.
If re-arrest occurs in a moving rig we pull over to perform CPR unless the ER can be reach in a couple of minutes. CPR quality and responder safety are at risk to do otherwise.
ACLS says
Hi Mark,
Thank you so much for sharing the information!
Kind regards, Jeff