 Integrated post-cardiac arrest care is the 5th link in the AHA adult chain of survival. Topics of focus for post-cardiac arrest care include temperature control, hemodynamic and ventilation optimization, immediate coronary reperfusion with PCI (percutaneous coronary intervention), glycemic control, neurologic care and other technical interventions. To be successful, post-cardiac arrest care requires an integrated multidisciplinary approach.
Integrated post-cardiac arrest care is the 5th link in the AHA adult chain of survival. Topics of focus for post-cardiac arrest care include temperature control, hemodynamic and ventilation optimization, immediate coronary reperfusion with PCI (percutaneous coronary intervention), glycemic control, neurologic care and other technical interventions. To be successful, post-cardiac arrest care requires an integrated multidisciplinary approach.
For the purposes of this site, the review of post-cardiac arrest care interventions will focus primarily on immediate post-arrest interventions and aspects that you will most likely be tested on.
For a complete review of the subject refer to your AHA provider manual. (pages: 150-158)
Temperature Control
Temperature control which was previously called TTM (targeted temperature management) is the only intervention that has been shown to improve neurological outcomes after cardiac arrest. Temperature control should occur soon after ROSC (return of spontaneous circulation) for all cardiac arrest patients, and should be maintained for 36 hours. The decision point for the use of temperature control is whether or not the patient can follow commands. (lack of meaningful response to verbal commands)
Temperature control includes choosing one temperature between 32-37.5 °C (89.6-97.5 °F) and then holding that temperature for at least 36 hours. Common methods used for maintaining temperature control are endovascular catheter, surface cooling devices, or other simple surface cooling interventions.
During induced temperature control, the patient’s core temperature should be monitored with any one of the following: esophageal thermometer, a bladder catheter in the nonanuric patients, or a pulmonary artery catheter if one is already in place.
Axillary and oral temperatures are inadequate for monitoring core temperatures.
Ventilation Optimization
During the post-cardiac arrest phase, inspired oxygen should be titrated to maintain an arterial oxygen saturation of ≥90-98%. The goal is to avoid hypoxia and hyperoxia. This reduces the risk of oxygen toxicity. Excessive ventilation should also be avoided because of the potential for reduced cerebral blood flow related to a decrease in PaCO2 levels. Also, excessive ventilation should be avoided because of the risk of high intrathoracic pressures which can lead to adverse hemodynamic effects during the post-arrest phase.
Quantitative waveform capnography can be used to regulate and titrate ventilation rates during the post-arrest phase. Visit the link for more details about waveform capnography.
Avoid excessive ventilation. Ventilation should start at 10/min and should be titrated according to the target PETCO2 of 35-45 mmHg.
Hemodynamic Optimization
Hypotension, a systolic blood pressure < 90 mmHg should be treated and the administration of fluids and vasoactive medications can be used to optimize the patient’s hemodynamic status. While the optimal blood pressure during the post-cardiac arrest phase is not known, the primary objective is adequate systemic perfusion, and a mean arterial pressure of ≥ 65 mmHg should accomplish this. A mean arterial pressure ≥ 65 mmHg should be maintained during the post-cardiac arrest phase.
The goal of post-cardiac arrest care should be to return the patient to a level of functioning equivalent to their prearrest condition.
IV infusions for the control of post-arrest hypotension:
- IV Fluid Bolus: Give 1-2 L of normal saline or LR
- Epinephrine 2-10 mcg/min
- Dopamine 5-20 mcg/kg/min
- Norepinephrine 0.1-0.5 mcg/kg/min
Other considerations
Moderate glycemic control measures should be implemented to maintain glucose levels within a normal range, and since there is an increased risk for hypoglycemia, attention should be focused on prevention. No specific glycemic target range is recommended at this time.
Every effort should be made to provide coronary reperfusion (PCI), and interventions should be directed with this goal in mind. PCI has been shown to be safe and effective in both the alert and comatose patient, and hypothermia does not contraindicate PCI.
Click below to view the Post-Cardiac Arrest Algorithm Diagram. When finished, click again to close the diagram.
Post-Cardiac Arrest diagram
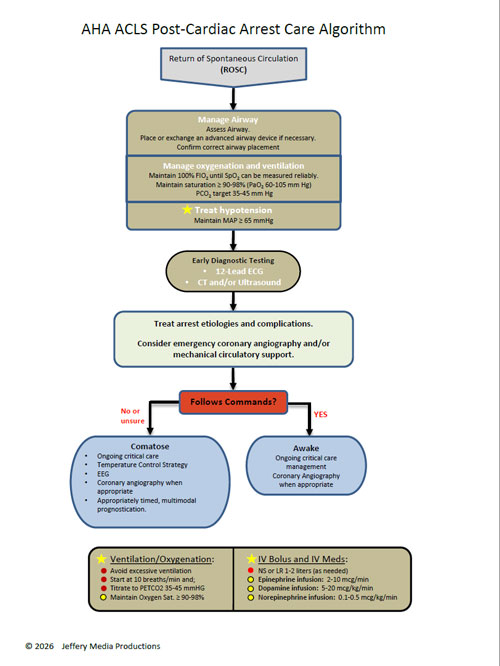
or Download the High Resolution PDF Here. (This will open in another window.)
osugo2012 says
We do code freeze post arrest and we do use ice until femoral line is placed then we use chilled saline.
ladrieme says
Hi Jeff,
I was interested in the therapeutic hyopthermia content, more specifically the method of inducing hypothermia. I know that in our institution we generally place patients on a cooling blanket, administer a paralytic agent (to prevent shivering), while they are intubated and sedated. I don’t think we have ever used ice cold IV fluids, is this considered to be more effective? Maybe our practice is outdated? Any thoughts?
Jeff with admin. says
I do think that either method of inducing hypothermia will work. However, using IV fluids to decrease core temperature would be much quicker than using a cooling blanket.
I would consider using IVF to be more effective for rapidly reducing the temp, but for temperature maintenance, the cooling blanket would be more practical at the bedside. It may be that a combination of both would be the best choice.
Kind regards,
Jeff
ryan2burke says
Took the resort acls. Passes w/o issues. The instructor stated that if you give the vasopressin dose instead of the first or second epi that you had to wait 30 mins before the next epi- that to me is like saying if the vasopressiin d/n work that’s all folks. My site d/t provide me with materials to study, but the book a co-worker had did not say this anywhere. ACLS is suppose to provide a standard set of protocols . The only time I have used vasopressin- and it’s a pain because the dose calls for 2 vials – the pt survived for long enough that his family got to say goodbye. I would think that not increasing oxygen demand while increasing vasoconstriction would ake vasopressin a better drug for suspected mi and people are already less likely to use the less familiar drug. What is the protocol?
Jeff with admin. says
What your instructor said about waiting 30 min. to give epinephrine is incorrect. Vasopressin can be given as a one time dose to replace the 1st or 2nd dose of epinephrine. You would use it as a direct replacement within the protocol. Then you would continue with the epinephrine every 3-5 minutes.
There is no clinical evidence that the use of epinephrine or vasopressin, when used during cardiac arrest, increase rates of survival to discharge from the hospital. However, studies have shown that epinephrine and vasopressin improve rates of ROSC (return of spontaneous circulation). —Kind regards, Jeff
Mary Anne Brady says
I have been ACLS certified for 12 years. I guess some life stressors had me more distracted than I thought and I failed the test but nailed the megacode. So, this site was recommended to me so I could study and retake the test. I posted below a quote from up above on this page…. This was a specific test question that I got wrong. I chose increased intrathoracic pressure as the answer and they told me that the correct answer was to prevent gastric distension. From a testing perspective…any thoughts? When I tried to argue the question they said that these answers were from AHA and my facility would not change any of them.
“Also, excessive ventilation should be avoided because of the risk of high intrathoracic pressures which can lead to adverse hemodynamic effects during the post arrest phase.”
So which is the better answer?
Dan says
Gatric distension occurs during bag mask ventilation. A properly located ET tube should produce no gastric distension unless the patient has a TE fistula. Good luck with your test.
mtoledo says
According to the AHA ACLS provider manual (AAPM), pg 38, under Critical Concepts: Avoiding Excessive Ventilation it states “Excessive ventilation can be harmful because it increases intrathoracic pressure, decreases venous return to the heart, and diminishes cardiac output. It may also cause gastric inflation and predispose the patient to vomiting and aspiration of gastric contents.” While on pg 75 under Caution: Things to Avoid During Ventilation it reads “Excessive ventilation may potentially lead to adverse hemodynamic effects when intrathoracic pressures are increased and because of potential decreases in cerebral blood flow when PaCO2 decreases”. IMHO, the AAPM seems to put more emphasis on intrathoracic pressures than gastric distention yet both are considered valid reasons to avoif excessive ventilation. Best of luck.
Vita Miller says
Just took the renewal class today and passed. The megacode was not really challenging because I have taken ACLS at least 10 times already. The test questions were somewhat trickier, but fortunately our instructor gave us clues throughout the course about the more difficult ones. Your website has been extremely useful as a study guide and I will certainly recommend it to my nurse colleagues.
cecelia says
So, tell us…how did you do on your test? Were the questions similiar to info covered at this site?
Jeff with admin. says
I had to certify last September under the new guidelines. I missed 1 on the exam and aced the Megacode. The questions on the exam were all covered in some way or another on the site. —Kind regards, Jeff
LISA LAL says
Starting to prepare for the exam. Very anxious to see how your questions compare to the real exam! The information appears great so far. Glad I found your web site!
Jodi Levy says
Great site. The practice tests were very helpful. I took the ACLS exam today and passed! Some of the questions found here were VERY similar to those on the actual test. The videos and megacode simulations were excellent too. Very helpful. THANKS!
Todd Penkala says
awesome, takes the pain out of preparing for re certification.
patricia a blake says
this site is and excellent review. Will be taking my ACLS recertification tomorrow and feel well prepared for the written test and mega code. Thanks
BEVERLY says
THIS AN ABSOLUTE AMAZING SITE.
Jeannine Piet-Roy says
The post cardiac care is informational Thank you
carole settembro says
This is one of the best ACLS sites. Thank you!!!!
Eulalie says
Thanks a lot! This site is great, I love it!!!!
LISA says
WHAT A GREAT SITE. THANKS
Debbie Ousley says
Thank you very much for this site! It has helped alot!