
SVT is a broad term for a number of tachyarrhythmias that originate above the ventricular electrical conduction system (Purkinje fibers).
Classic Paroxysmal SVT has a narrow QRS complex & has a very regular rhythm. Inverted P waves are sometimes seen after the QRS complex. These are called retrograde p waves.
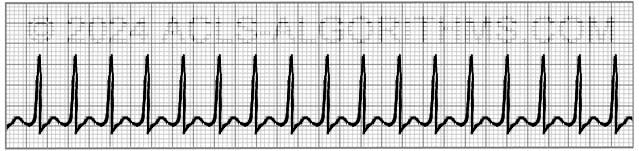
The heart fills during diastole, and diastole is normally 2/3 the cardiac cycle. A rapid heart rate will significantly reduce the time which the ventricles have to fill. The reduced filling time results in a smaller amount of blood ejected from the heart during systole. The end result is a drop in cardiac output & hypotension.
With the drop in cardiac output, a patient may experience the following symptoms. These symptoms occur more frequently with a heart rate >150 beats per minute:
- Shortness of air (S)
- Palpitation feeling in chest (S)
- Ongoing chest pain (U)
- Dizziness (S)
- Rapid breathing (S)
- Loss of consciousness (U)
- Numbness of body parts (S)
The pathway of choice for SVT in the tachycardia algorithm is based on whether the patient is stable or unstable. The symptoms listed above that would indicate the patient is unstable are noted with the letter (U). Stable but serious symptoms are indicated with the letter (S).
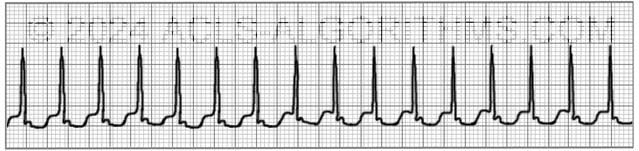
Unstable patients with SVT and a pulse are always treated with synchronized cardioversion. The appropriate voltage for cardioverting SVT is 50-100 J. This is what AHA recommends and also SVT converts quite readily with 50-100 J.
Below is a short video which will help you quickly identify supraventricular tachycardia on a monitor.
Please allow several seconds for the video to load. (4.37 mb)
Click for next Rhythm Review: Atrial Flutter
Questions Asked On This Page
-
Q: What are vagal maneuvers?
A: A vagal maneuver is a technique by which you attempt to increase intrathoracic pressure which stimulates the vagus nerve. This can result in slowed conduction of electrical impulses through the AV node of the heart. The following methods can be used.- Cough Method: Have a patient cough forcefully. This is a simple form of vagal maneuver. A cough stimulates an increase in intrathoracic pressure which will stimulate the vagus nerve. This can result in slowed conduction of electrical impulses through the AV node of the heart.
- Straw Method: Have the patient blow forcefully through a straw for 3-5 seconds.
- Bear down Method: Have the patient bear down and strain. Kind of like how a person might strain when having a bowel movement.
- Syringe Plunger Method: First, show the patient how easy it is to move the plunger by pulling it back and forth in within the syringe. Now instruct the patient place their mouth over the exit end of the syringe and attempt to blow the plunger out of the syringe. Have them blow for 3-5 seconds.
- Abdominal Pressure Method: Press into the patient’s abdomen while they contract and resist pressing into their abdomen.
- Ice Method: Quote from a healthcare provider: “We had a kid (approximately 12 yrs old) present to our ER in SVT, instead of using drugs and vagal maneuvers we dunked his face in a bucket of ice twice, and it immediately & effectively brought the heart rate down. We observed him for a period of time, and the kid was fine. Worked wonders! Young army doctor’s idea!”
-
Q: I can’t distinguish the sinus tachycardia example from the three re-entry SVT examples on the pre-test no matter how long I stare at the strips…they look identical to me. Help please, and thanks.
A: On the Pretest at the AHA website, Look at each image carefully. Don’t try to over-observe. Just look at each one and notice how many QRS complexes there are.
There are almost double the amount of QRS complexes in all of the SVT when compared to the Sinus Tachycardia. This is the easiest way to tell SVT from Sinus tachycardia. Also, P-waves are only clear in the sinus tachycardia. Most of the time with SVT you will not be able to see the p-waves. SVT rate will usually be greater than 150 and Sinus tachycardia will be less than 150. -
Q: Let me get this straight. Svt is a heart rate greater than 150 with conduction at or above the av node?
A: That is correct.
Susan Delahanty says
This is my first time studying for ACLS. And I see “Shock” “Defib” and “Cardioversion”. Are all these the same thing?
Sorry if this is a basic question. But they all seem the same to me. We put the pads on and hit the button.
Thank you
ACLS says
Defibrillation and cardioversion are different actions. They are both classified as a “shock” and the main factor is exactly when that shock can occur during the electrical conduction phase with of the heart.
This page on the site will give you a good understanding of the difference between defibrillation and synchronized cardioversion.
https://acls-algorithms.com/synchronized-and-unsynchronized-cardioversion/
To summarize, defibrillation is an emergency procedure used for patients in cardiac arrest, delivering a high-energy, unsynchronized shock to treat life-threatening arrhythmias like ventricular fibrillation. In contrast, cardioversion is a planned procedure for patients with a pulse, using a lower-energy shock to treat less severe arrhythmias such as atrial fibrillation. A key difference is that cardioversion is synchronized meaning the shock is delivered at a very specific time in the heart’s electrical conduction cycle, typically during the R wave of the QRS complex, to avoid inducing more dangerous arrhythmias. While both involve delivering an electrical shock to the heart, they differ in their urgency, energy levels, synchronization with the heart’s rhythm, and the types of arrhythmias they treat.
Kind regards,
Jeff
Mlandeli J Ncube says
Enjoyed reading the. It helped.
Jess says
What if the patient has unstable SVT but only defibrillator is available?
ACLS says
If a patient has unstable SVT in a defibrillator is available you can perform synchronized cardioversion.
Kind regards,
Jeff
Nicholas says
I was taught SVT was 120-150bpm, with Atach being 150+. Is this wrong?
ACLS says
Yes, this is wrong. Typically SVT will have a rate greater than 150/min. Typical rates are between 150-200 per minute.
Kind regards,
Jeff
gladys pena says
how can you differentiate between SVT and wolf Parkinson syndrome. I nursed a patient with a tachycardia of 213 bp per mint and conscious with nil symptoms or drop in its haemodynamic
Jeff with admin. says
Determining whether the patient has WPW is done when the patient is not tachycardic. While the patient is tachycardic there is no way to determine. Patients with WPW will have a qrs complex that has “slurring” on the initial R wave and the PR interval will be short.
On the following website, you will find a diagram in a box titled:
“ECG features of WPW in sinus rhythm”
this will give you a good example of what to look for with regard to WPW. Wolff-Parkinson White syndrome
Kind regards,
Jeff
RHulse says
No PR interval on WPR; that’s why QRS is slurred. Impulse goes straight to the Purkinje fibers.
RHulse says
WPW, WPR
Kristin Nelson says
Will there be a RHYTHM section on the ACLS test?
Jeff with admin. says
There is not a designated section for rhythm identification, but there will be questions on the written exam that require you to be able to identify all of the major arrhythmias.
Kind regards,
Jeff
Bonnie Villarreal says
Just FYI…I was found to have an extra AV node after a couple of episodes of SVT through EP. No treatment was needed as I could usually convert with a vagal manuever and rest. I am a survivor of a rare form of pancreatic cancer. Chemo appeared to attack that AV node and I went through several treatments of SVT in the ER and, finally, a cardiac ablation. The best way I can describe it is, you are running very rapidly and then with a dose of Adenosine, you hit the proverbial brick wall. It always took the second dose for me, and it’s important to flush immediately and raise the affected IV site arm. Working on 13yrs of survival and no further SVT.
Just found your course, and it’s AWESOME! Thank you!
Jeff with admin. says
Thanks for sharing your story. I’m so glad that you haven’t had any more reoccurrences of SVT.
Thanks the Lord for your healing from pancreatic cancer as well.
Kind regards,
Jeff
Amber Mitchell says
Do you sedate and synchronize cardio RRT?
Jeff with admin. says
I’m not sure what the abbreviation you are using means. Can you clarify your question.
Kind regards,
Jeff
Brett says
A patient comes into the Emergency room with a heart rate of 180. (Svt)
Adenosine is given at 6mg. The first dose doesn’t work so a 12mg dose is administered and nothing. Doctor decides to do synchronized cardioversion at 50j.
Patient goes into atrial flutter. A second cardioversion is done at 100j. Nothing is bringing the patients heart rate down.
After 2nd cardioversion is done patient goes unconscious and is still in atrial flutter.
What could be going on here? Patient was clean with no drugs in system.
Jeff with admin. says
My first thought is “was it really SVT?” Without more assessment and history and a look at the 12-lead ECG, I have no idea. Nothing else comes to mind with the info provided.
If the patient was stable, I would not have attempted cardioversion. I would have attempted to get a cardiologist to evaluate the patient.
Kind regards,
Jeff
Brian says
Uncontrolled A-Fib…of course adenosine won’t work….should palpate a radial or some pulse and not read from monitor….A-Fib and SVT get mixed up a lot…….my thoughts ….I have been in the prehospital for 18 years…medic for 11….
Katherine Hogan says
What happened to Adenocard in the algorithm?
Jeff with admin. says
Adenocard (adenosine) it’s still part of the tachycardia algorithm. All of this information is covered on the site pages that review the tachycardia algorithm.
Kind regards,
Jeff