 The major ECG rhythms classified as bradycardia include:
The major ECG rhythms classified as bradycardia include:
- Sinus Bradycardia
- First-degree AV block
- Second-degree AV block
- Type I —Wenckebach/Mobitz I
- Type II —Mobitz II
- Third-degree AV block complete block
Bradycardia vs. Symptomatic Bradycardia
Bradycardia is defined as any rhythm disorder with a heart rate less than 60 beats per minute. (Usually less than 60)
Symptomatic bradycardia, however, is defined as a heart rate less than 60/min that elicits signs and symptoms, but the heart rate is typically less than 50/min.
Symptomatic bradycardia exists when the following 3 criteria are present: 1.) The heart rate is slow; 2.) The patient has symptoms, and 3.) The symptoms are due to the slow heart rate.
Relative bradycardia occurs when a patient may have a heart rate within normal sinus range, but the heart rate is insufficient for the patient’s condition. An example would be a patient with a heart rate of 80 bpm when they are experiencing septic shock.
Bradycardia Pharmacology
There are 3 medications that are used in the Bradycardia ACLS Algorithm. They are atropine, dopamine (infusion), and epinephrine (infusion). More detailed ACLS pharmacology information is reviewed following this page.
- The single dose administration of atropine was increased from 0.5 mg to 1 mg. Now give 1 mg for the first dose and then repeat every 3-5 minutes at the 1 mg dose.
- Also, the dopamine infusion rate for chemical pacing was changed to 5-20 mcg/kg/min.
The previous rate from the 2015 guidelines was 2-20 mcg/kg/min. - The demand rate may be set at a range from 60-80/min. 2015 guidelines had the start demand rate to start at only 60/min.
2015 AHA Update: For symptomatic bradycardia or unstable bradycardia IV infusion a chronotropic agent (dopamine & epinephrine) is now recommended as an equally effective alternative to external pacing when atropine is ineffective.
Atropine: The first drug of choice for symptomatic bradycardia. The dose in the bradycardia ACLS algorithm is 1 mg IV push and may repeat every 3-5 minutes up to a total dose of 3 mg.
Dopamine: Second-line drug for symptomatic bradycardia when atropine is not effective. Dosage is 5-20 micrograms/kg/min infusion.
Epinephrine: Can be used as an equal alternative to dopamine when atropine is not effective. Dosage is 2-10 micrograms/min.
Bradycardia Algorithm
The decision point for ACLS intervention in the bradycardia algorithm is determination of adequate perfusion. For the patient with adequate perfusion, observe and monitor the patient. If the patient has poor perfusion, preparation for transcutaneous pacing should be initiated, and an assessment of contributing causes (H’s and T’s) should be carried out.
Click below to view the bradycardia algorithm diagram. When finished, click again to close the diagram.
Bradycardia Algorithm Diagram
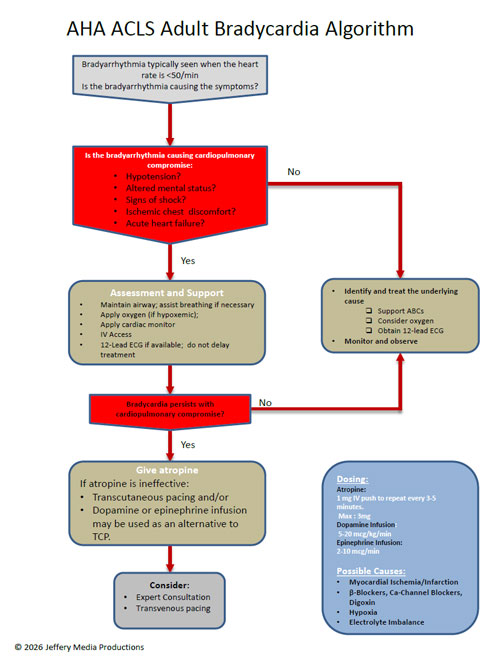
or Download the High Resolution PDF Here. (This will open in another window.)
Transcutaneous pacing (TCP)
Preparation for TCP takes place as atropine is being given. If atropine fails to alleviate symptomatic bradycardia, TCP is initiated. Ideally, the patient receives sedation prior to pacing, but if the patient is deteriorating rapidly, it may be necessary to start TCP prior to sedation.
For the patient with symptomatic bradycardia with signs of poor perfusion, transcutaneous pacing is the treatment of choice.
Do not delay TCP for the patient with symptomatic bradycardia with signs of poor perfusion. The starting rate for TCP is 60-80/min and adjust up or down based on the patient’s clinical response. The dose for pacing is set at 2mA (milliamperes) above the dose that produces observed capture.
TCP is contraindicated in the patient with hypothermia and is not a recommended treatment for asystole.
Do not use a carotid pulse check for the assessment of circulation as TCP can create muscular movements that may feel like a carotid pulse. Assess circulation using the femoral pulse.
Identification of contributing factors for symptomatic bradycardia should be considered throughout the ACLS protocol since reversing of the cause will likely return the patient to a state of adequate perfusion.
Top Questions Asked on This Page
-
Q: Should I use atropine in all cases of symptomatic bradycardia regardless of the level of block? The prep test for AHA ACLS seems to support giving atropine initially in symptomatic second-degree block type II, but not for complete block.
A: There are a couple of things to mention here. First, atropine may be used for any type of block but may negatively affect outcomes if the bradycardia is being caused by myocardial infarction.
This negative effect may occur because atropine increases the heart rate and myocardial oxygen demand. In the case of bradycardia caused by MI, it would be safer to transcutaneous pace (TCP) at a rate of 60 and move toward some type of cardiac intervention. You should use the 12 lead ECG to help determine MI. This will help determine if atropine may exacerbate the patient’s condition. If the patient has severe symptoms, you should not delay transcutaneous pacing (TCP).
You will usually have time to try atropine as you prepare for TCP.
Second, AHA states “For Mobitz II and complete block (3rd Degree block), atropine should not be relied upon.” This does not mean that it is contraindicated. It just means that it should not be relied upon because there is a good chance that it will not work.
It may not work because atropine blocks the action of the vagus nerve. Atropine works at the SA and AV node through its effect on the vagus nerve, and since conduction abnormalities associated with 2nd-degree block type II and 3rd-degree heart block are below (distal) the site of action for atropine, the drug will typically have an insignificant effect.
-
Q: Why is pacing contraindicated in hypothermia?
A: Bradycardia may be physiologic in the hypothermic patient. This type of bradycardia is an appropriate response to the decreased metabolic rate that normally occurs with hypothermia.
Also the hypothermic ventricle is more prone to fibrillation with any sort of irritation. Thus the irritation of TCP could induce VF. Once the hypothermic ventricle begins to fibrillate, it is more resistant to defibrillation. Warm the patient and then treat any remaining arrhythmias.
-
Q: What is TCP?
A: TCP means transcutaneous pacing.
-
Q: What is chemical pacing?
A: Chemical pacing is when IV medications (epinephrine or dopamine) are used to increase the heart rate rather than the transcutaneous pacing which uses electricity to increase the heart rate.
sushama francis says
Hi,
What medication is given for sedation prior to TCP?
Great site, thanks!!
sushama
Jeff with admin. says
Versed and ativan are probably the most common, but there are many others that could be used. I suppose it depends on the facility and what they stock.
vivian Anyanaso says
Simply beautiful site!.. if you love learning …you are in the right spot..Thx Jeff
Mohammed Al Zayer says
Hello,
is it enough to read from the site and ignore the book?
Jeff with admin. says
https://acls-algorithms.com/terms-of-use
Elizabeth Risner says
Hi, this goes to Respiratory arrest: I wasn’t able to comment on that page. What does perfusing rhythm mean? You said to give 1 breath every 5-6 seconds for it. Thank you
Jeff with admin. says
Thanks for the question.
Perfusing rhythm means that the electrical and myocardial contraction is sufficient
to deliver blood to the body and vital organs.
Kind regards,
Jeff
Elizabeth Risner says
What if your patient is apneic, and their heart rate is rapidly deacreaing to sinus bradycardia with 30 bpm? Which medication would you give?
Jeff with admin. says
atropine per the bradycardia algorithm. Jeff
Scarlett says
To Carlene Bradley and also to Jeff:
Thank you for the tips and assistance. I have ACLS coming up next month, so I am studying the books, this website etc. I appreciate your tip Carlene, about reassessing my patient when I need a little more time to find the correct answer. I am in a class where the instructors are so rough, they will make you cry. Students drop out very quickly. Last year, I think they only passed 2 students. You go the whole year passing the class then they fail you at ACLS. I have worked my whole life in the medical field and handled all types of emergencies very well, but these guys make me so nervous, I feel like they will be doing a code on me !
Ina says
Would there ever be a time when CPR is started for a patient with symptomatic bradycardia with a weak pulse? What if you don’t have a TCP and atropine doesn’t work?
Chris with admin. says
Hello ,
Great Question. All modern defibrillators should have the capability to transcutaneous pace. The only time that CPR should be performed is in the setting of cardiac arrest. If a patient has a pulse, chest compressions are actually contraindicated. From my experience with atropine and bradycardia, you will at least get a transient increase in heart rate. Other considerations would be to start a epinephrine drip or dopamine drip. Both of these drugs have good effect to increase heart rate. Chest compressions should only be performed in the setting of cardiac arrest. If the patient becomes pulseless then you can start chest compression. If breathing is ineffective at anytime, you can begin bag-mask ventilation.–Chris
Carlene Bradley says
Hey Scarlet, That’s a hard situation to be in. I can relate, I’ve been a Paramedic since 1994, back when the instructors seemed to relish making ACLS hell. My advise would be… It never hurts to state BSI and scene safety (good habit) also if your patient/monitor doesn’t do well, don’t let that rattle you, sometimes instructors will do that to “simulate” what happens in real life, so don’t take it as a sign that you ordered the wrong treatment, just deal with the new change and move on. Most important of all don’t get in a rush… if you feel stuck or lost just state ” I’d like to take a moment to reassess my patient” I’ve never seen anyone get in trouble for reassessing, checking for any change in the patient i.e. checking for pulse, still no pulse? etc. this is always good to do and will give you a little time to collect yourself.
You say most people there don’t pass, that would indicate to me that your instructors are not doing their jobs as well as they should or they are creating a stressful testing environment, which is no more then psychological warfare if you ask me, they justify it by saying that real life codes are more stressful, yes, but it’s a different kind of stress and I don’t agree with these type of testing tactics, I’ve seen people so freaked out during testing that I thought we’d have to work a code on them, seriously (pale diaphoretic) it’s uncalled for. So recognize what they are trying to do and just follow the algorithm that’s in your head. Hope this helps. Best wishes.
Scarlett says
Can anyone give me any tips or pointers on how to pass the ACLS based upon their recent experience with it? Anything you may have encountered during the ACLS that would help someone pass, etc. ?
I have to take it soon and the instructors are very hard nosed here. I have studied the books, studied the rhythms, etc. but if you miss one thing, they fail you and you are completely out of the class, losing a year’s work. Most people here do not pass it. Thank you for your help.
Denise Earles says
Wow! That sounds like a bad question, about the 3rd HB. Whenever looking at a rhythm we must also always always look at the patient. To make a decision on that question of the 3rd HB we need to know the signs and symptoms of the patient. And if my patient was in that rhythm and symptomatic I would call a code before he dies, not rapid response and end up calling a code anyway when he does die.
Kiansu says
3rd Degree Heart Block Question(HELP)
TEST Question: Shows a 3rd HB Strip ONLY! Nothing else on the strip that indicates pts condition of Symptomatic or Non Symptomatic. However noted in study packet and have been informed and constantly reminded and drilled that 3rd HB is a LETHAL Rhythm. Made mention on numerous, numerous times of the 5 lethal (VF/Pulseless VT, PEA,Astoyle and 3rd HB
NI:Get some help, call a code, begin cpr, epi (Nurse treats it as a critical lethal rhythm 1st)
TPM,PPM and or TQP (Nurse indicates all these interventions) Instructor fails students due to calling a code and not a rapid response, beginning cpr and giving epi basically for treating the pt critically….Are Nursing interventions Wrong and requires failure and 3 day EKG class and Must pass next exam or out of the program….REALLY? Treating pt critically and lethally?
Jeff with admin. says
First let me try and interpret what you said so I can make sure that I am answering your question: You are saying that you treated 3rd degree block by calling a code, beginning cpr and giving epi.
3rd degree block CAN be a lethal rhythm, but many times a patient might be in a 3rd degree block and not be symptomatic. I have seen this myself.
You should follow the bradycardia algorithm when treating bradycardia. Here is a link to the AHA ACLS Bradycardia algorithm: http://circ.ahajournals.org/content/122/18_suppl_3/S729/F3.large.jpg
As you can see in the algorithm, Step 3. The decision point for treating bradycardia or monitoring is based on symptoms. If the patient has persistent symptoms from the bradycardia/bradyarrhythmia then you will treat by following the bradycardia algorithm. If not you monitor/observe.
It would be very appropriate to active a rapid response team if you saw someone with a 3rd degree block on a monitor. 3rd degree block has a high likelihood of degrading into a lethal rhythm or a symptomatic bradycardia.
Kind Regards,
Jeff
Dana Maes says
It is always good to have reminders and prompts as we do not have code situations that often on our floor.
Mary J Irving says
I do so appreciate your reply so quickly. Since so much has changed with acls, it is nice to have the medication dosage on hand to for me.
heidi aleman says
Question- what does AHA say about atropine and 3rd degree HB
jeff with admin. says
3rd Degree HB is treated per the algorithm. Fist intervention can be atropine 0.5mg IV. However, AHA pg. 111 says this “do not rely on atropine in Mobitz Type II second-or third-degree AV block or in patients with 3rd degree aV block with a new wide QRS complex.” It does not mean that you can’t give it, but it does mean that you would not want the administration of atropine to delay TCP if the patient is showing signs of poor perfusion.
jeff with admin. says
Also AHA page 111 states: “healthcare providers should consider immediate pacing in UNSTABLE patients with high degree heart block when IV access is not available.
rafik says
It is the best site where we can learn and known every thing in ACLS, thank you , and I am very happy to discover this site. good luck for every one