 The major ECG rhythms classified as bradycardia include:
The major ECG rhythms classified as bradycardia include:
- Sinus Bradycardia
- First-degree AV block
- Second-degree AV block
- Type I —Wenckebach/Mobitz I
- Type II —Mobitz II
- Third-degree AV block complete block
Bradycardia vs. Symptomatic Bradycardia
Bradycardia is defined as any rhythm disorder with a heart rate less than 60 beats per minute. (Usually less than 60)
Symptomatic bradycardia, however, is defined as a heart rate less than 60/min that elicits signs and symptoms, but the heart rate is typically less than 50/min.
Symptomatic bradycardia exists when the following 3 criteria are present: 1.) The heart rate is slow; 2.) The patient has symptoms, and 3.) The symptoms are due to the slow heart rate.
Relative bradycardia occurs when a patient may have a heart rate within normal sinus range, but the heart rate is insufficient for the patient’s condition. An example would be a patient with a heart rate of 80 bpm when they are experiencing septic shock.
Bradycardia Pharmacology
There are 3 medications that are used in the Bradycardia ACLS Algorithm. They are atropine, dopamine (infusion), and epinephrine (infusion). More detailed ACLS pharmacology information is reviewed following this page.
- The single dose administration of atropine was increased from 0.5 mg to 1 mg. Now give 1 mg for the first dose and then repeat every 3-5 minutes at the 1 mg dose.
- Also, the dopamine infusion rate for chemical pacing was changed to 5-20 mcg/kg/min.
The previous rate from the 2015 guidelines was 2-20 mcg/kg/min. - The demand rate may be set at a range from 60-80/min. 2015 guidelines had the start demand rate to start at only 60/min.
2015 AHA Update: For symptomatic bradycardia or unstable bradycardia IV infusion a chronotropic agent (dopamine & epinephrine) is now recommended as an equally effective alternative to external pacing when atropine is ineffective.
Atropine: The first drug of choice for symptomatic bradycardia. The dose in the bradycardia ACLS algorithm is 1 mg IV push and may repeat every 3-5 minutes up to a total dose of 3 mg.
Dopamine: Second-line drug for symptomatic bradycardia when atropine is not effective. Dosage is 5-20 micrograms/kg/min infusion.
Epinephrine: Can be used as an equal alternative to dopamine when atropine is not effective. Dosage is 2-10 micrograms/min.
Bradycardia Algorithm
The decision point for ACLS intervention in the bradycardia algorithm is determination of adequate perfusion. For the patient with adequate perfusion, observe and monitor the patient. If the patient has poor perfusion, preparation for transcutaneous pacing should be initiated, and an assessment of contributing causes (H’s and T’s) should be carried out.
Click below to view the bradycardia algorithm diagram. When finished, click again to close the diagram.
Bradycardia Algorithm Diagram
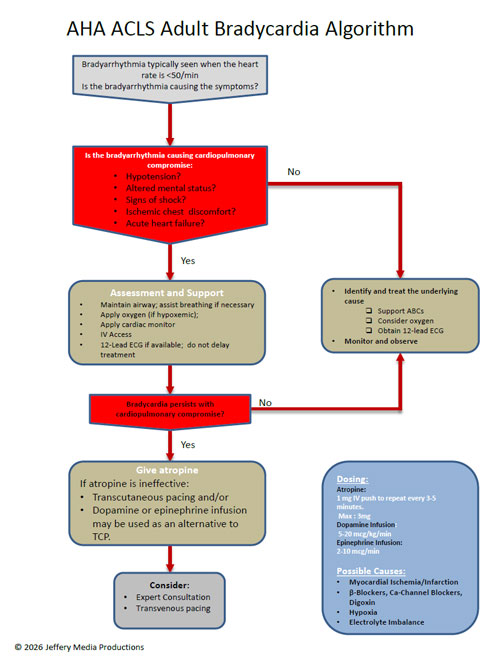
or Download the High Resolution PDF Here. (This will open in another window.)
Transcutaneous pacing (TCP)
Preparation for TCP takes place as atropine is being given. If atropine fails to alleviate symptomatic bradycardia, TCP is initiated. Ideally, the patient receives sedation prior to pacing, but if the patient is deteriorating rapidly, it may be necessary to start TCP prior to sedation.
For the patient with symptomatic bradycardia with signs of poor perfusion, transcutaneous pacing is the treatment of choice.
Do not delay TCP for the patient with symptomatic bradycardia with signs of poor perfusion. The starting rate for TCP is 60-80/min and adjust up or down based on the patient’s clinical response. The dose for pacing is set at 2mA (milliamperes) above the dose that produces observed capture.
TCP is contraindicated in the patient with hypothermia and is not a recommended treatment for asystole.
Do not use a carotid pulse check for the assessment of circulation as TCP can create muscular movements that may feel like a carotid pulse. Assess circulation using the femoral pulse.
Identification of contributing factors for symptomatic bradycardia should be considered throughout the ACLS protocol since reversing of the cause will likely return the patient to a state of adequate perfusion.
Top Questions Asked on This Page
-
Q: Should I use atropine in all cases of symptomatic bradycardia regardless of the level of block? The prep test for AHA ACLS seems to support giving atropine initially in symptomatic second-degree block type II, but not for complete block.
A: There are a couple of things to mention here. First, atropine may be used for any type of block but may negatively affect outcomes if the bradycardia is being caused by myocardial infarction.
This negative effect may occur because atropine increases the heart rate and myocardial oxygen demand. In the case of bradycardia caused by MI, it would be safer to transcutaneous pace (TCP) at a rate of 60 and move toward some type of cardiac intervention. You should use the 12 lead ECG to help determine MI. This will help determine if atropine may exacerbate the patient’s condition. If the patient has severe symptoms, you should not delay transcutaneous pacing (TCP).
You will usually have time to try atropine as you prepare for TCP.
Second, AHA states “For Mobitz II and complete block (3rd Degree block), atropine should not be relied upon.” This does not mean that it is contraindicated. It just means that it should not be relied upon because there is a good chance that it will not work.
It may not work because atropine blocks the action of the vagus nerve. Atropine works at the SA and AV node through its effect on the vagus nerve, and since conduction abnormalities associated with 2nd-degree block type II and 3rd-degree heart block are below (distal) the site of action for atropine, the drug will typically have an insignificant effect.
-
Q: Why is pacing contraindicated in hypothermia?
A: Bradycardia may be physiologic in the hypothermic patient. This type of bradycardia is an appropriate response to the decreased metabolic rate that normally occurs with hypothermia.
Also the hypothermic ventricle is more prone to fibrillation with any sort of irritation. Thus the irritation of TCP could induce VF. Once the hypothermic ventricle begins to fibrillate, it is more resistant to defibrillation. Warm the patient and then treat any remaining arrhythmias.
-
Q: What is TCP?
A: TCP means transcutaneous pacing.
-
Q: What is chemical pacing?
A: Chemical pacing is when IV medications (epinephrine or dopamine) are used to increase the heart rate rather than the transcutaneous pacing which uses electricity to increase the heart rate.
Laura1 says
I did my acl s and aced it but I do have a question. On the Brady algorithm it says epi and dopamine drips. When I did the megacode the instructor said after the atropine the next drug would be epi 1 mg,which makes sense but I went by the algorithm. Are both correct options?
Laura1 says
Epi 1mg ivp is what I was told,not the drip
Jeff with admin. says
This is incorrect. See previous email for the details. Your instructor was providing you with information that is not accurate.
Kind regards,
Jeff
Jeff with admin. says
Epinephrine 1 mg IV PUSH is not recommended within the bradycardia algorithm. I’m not sure why your instructor provided this information.
However, when you mix an epinephrine drip it is typically mixed 1 mg in 500 ml of NS or D5W. Then the infusion should run at 2-10 micrograms/min (titrated to effect).
Kind regards,
Jeff
Laura1 says
Ty. That’s what I thought,according to the algorithm but I wasn’t going to say otherwise since she ran the megacode.
Aaron says
Can you use the TCP method for bradycardia without symptoms?
Jeff with admin. says
You can and this would be under the discretion of the provider. It would be outside of following the AHA ACLS guidelines and you would want to have a clear and justifiable reason for pacing.
There are other interventions that should be considered for asymptomatic bradycardia.
Kind regards,
Jeff
Parham says
Hi ; If the patient has AF rhythem , and also bradycardia , which drug can be our choice ?
Jeff with admin. says
Symptoms related to AF are usually seen when the AF is present with a rapid ventricular rate. If a patient is symptomatic and profound bradycardia is present with an underlying AF then you would most likely treat with atropine initially. Most important would be to identify what is causing the bradycardia and treat that.
Kind regards,
Jeff
MM says
If a patient is in 3degree HB with a HR of 13 and you are alone at the bedside should CPR be initiated?
Jeff with admin. says
If you are alone at the bedside with an adult patient who has a palpable pulse of 13 bpm and is unconscious or unstable you should:
1. Call for help and a defibrillator
2. Open the airway/assist breathing
3. Apply O2 (if available)
4. Apply a cardiac monitor (if available)
5. Give atropine (if available)
6. Chest compressions are not part of the bradycardia algorithm, but with such profound bradycardia in an unconscious patient, chest compressions would be an acceptable alternative for improving blood perfusion. Until help arrives and other interventions can be provided.
Make sure that you are searching for a cause of the bradycardia as well. H and T’s.
Remember: AHA says: “The healthcare provider can tailor interventions to achieve the best outcome.”
Kind regards,
Jeff
Craig Di Leo says
No Atropine for 2 degree type II and 3 degree Heart block. I don’t see this emphasized in the above algorithm.
Jeff with admin. says
There is nothing in the algorithm that says atropine is not given for second-degree type II and 3rd° block.
American Heart Association Guidelines say do not rely on atropine for the treatment of 2nd° block type II and 3rd° block. It is unlikely that 2nd° block and 3rd° block will be affected by the use of atropine.
This is because atropine works at the level of the AV node and often times 2nd° block type II and 3rd° block originate below the level of the AV node.
If a patient is not unstable (Poor perfusion) then atropine can be attempted in most cases of 2nd° black type II 3rd° block. Just realize that it may not work and transcutaneous pacing needs to be considered and prepared for.
Kind regards,
Jeff
Roula says
I am a nurse and I found this web site very helpful . The explanations given are clear and direct . Thank you.
LH says
If a patient was hypothermic. Are these algorithms the same?
Jeff with admin. says
Yes, the algorithm would be the same, but the hypothermia would be treated as one of the H of the H and T’s. It would be a given that the prime objective would be reversing the hypothermia in order to adequately treat the bradycardia.
Kind regards,
Jeff
Talat Mahmood says
A few questions. Please reply.
1) when there is delay in TCP, Can we give adrenaline infusion in cases where atropine did not improve symptomatic bradycardia?
2) If patient is deteriorating quickly and atropine did not work, can we give adrenaline as a slow bolus to terminate bradycardia to save the life of the patient?
3) Is there a place for adrenaline after failure of response to atropine when TCP is available?
Jeff with admin. says
1.) Yes
2.) Give the epinephrine as in infusion. Following the bradycardia algorithm
3.) if a patient remains hypotensive after the initiation of transcutaneous pacing, adrenaline (epinephrine) may be beneficial for improving hypotension.
Kind regards,
Jeff
Nathaniel says
After pacing, does the infusion rate of adrenaline still remain 2-10 micrograms?
Jeff with admin. says
If the epinephrine is being used for rate control then the raid would be 2-10 mcg per min.
Kind regards,
Jeff
Rachel Jolokai says
One box says new 2015 AHA standards say that dopamine and Epinephrine are equal alternatives to TCP. The next box then says TCP is the tx of choice for symp. Brady. So are they equally good or should you always pick TCP over the drugs if atropine fails?
Jeff with admin. says
According to the American Heart Association guidelines, epinephrine and dopamine are considered equal alternatives to transcutaneous pacing. Any one of the above can be attempted with the same priority. If there is a lack of response with one, then another is attempted.
Kind regards,
Jeff
Caren says
Based on your experience with TCP, which pad placement provides more successful pacing, anterior-anterior or anterior-posterior? And at what mAh you usually achieve capture with your patients? Most defibs can go as high as 200 mAh but usually what is the common pacing threshold? Thanks!
by the way this website is very helpful. thumbs up.
Jeff with admin. says
Healthy individuals will typically have a pacing threshold that is less than 80 mAh.
I have always seen a high rate of success with anterior-posterior. The most important thing is that the pads are placed so that the heart is sandwiched directly between them.
Kind regards,
Jeff
Nadav says
Questions here,
Let’s say I have bardycardic patient with signs of poor perfusion.
1. Why not always use TCP? Isn’t it the safest and most reliable way to control bradycardia?
2. Are there scenarios where you’d prefer using dopamine/adrenaline over TCP?
Would love to hear you explanation,
Nadav
Jeff with admin. says
There maybe scenarios when transcutaneous pacing does not work for a patient. Capture may be unattainable for ineffective to restore adequate perfusion. In this case, you would want to use the dopamine or epinephrine. In my professional opinion, I would always attempt TCP prior to using dopamine or epinephrine.
Does that make sense? If you have any other questions just let me know.
Kind regards,
Jeff
Nadav Shoua says
Got it. Thanks for your answer!
Parker says
Is it recommended at all to combine dopamine/epi with the TCP?
Jeff with admin. says
There are no recommendations for the use of dopamine and epinephrine (for rate control) to be used together with TCP. There may be times when dopamine or epinephrine could be used to improve blood pressure. In these cases, the dosing for blood pressure control would be different than the dosing used for heart rate control.
Kind regards,
Jeff
Nathaniel says
What would be the infusion rate for adrenaline in such instance?
Jeff with admin. says
The dosing for an epinephrine infusion to control blood pressure is typically 0.1-0.5 mcg/kg per min. (In 70 kg adult: 7-35 mcg per min)
This is in contrast to the dosing of an epinephrine infusion for heart rate control which is 2-10 mcg/min
Kind regards,
Jeff
Ante Santic says
Hi Jeff,
if I need give epinephrine 2-10 mcg/min or dopamine 2-20 mcg/kg/min infusion with how much NS (I guess with NS) will dilute. And how long we need give infusion.
Best regards
Jeff with admin. says
IV infusion for bradycardia:
Epinephrine: 1mg epinephrine is mixed with 500ml of NS or D5W. The infusion should run at 2-10 mcg/min and titrate to the patient’s response.
Dopamine: 400 mg dopamine is mixed with 250 ml NS. Begin the dopamine infusion at 2 to 20 mcg/kg/min and titrate to the patient’s response.
Larissa says
Hi Jeff let me know if it is right approach for symptomatic bradycardia, to apply transcutaneous pace maker to patient who’s permanent pacemaker is malfunctioning and is occasionally not capturing when fires . Is it going to be a some kind of conflict between external and internal pacemakers?
Thank you. Larissa
Jeff with admin. says
You can TCP right over the malfunctioning pacemaker and then get ahold of the manufacturer as soon as possible. Once the external pacemaker has captured and is providing the electoral impulse for the heart, the internal pacemaker should stop sensing the need to fire.
Just make sure that you do not pace the pacing patches directly over the internal pacemaker.
Kind Regards,
Jeff
Ishaan says
What all can happen in case of a suboptimal dose of atropine? Suppose a 0.3 mg dose is given initially?
Jeff with admin. says
Worst case scenario, atropine when given low dose can have a paradoxical effect and exacerbate bradycardia.
Best case scenario, the dose of atropine will not be high enough to increase the heart rate.
Kind regards,
Jeff
Kelly says
Do you administer the dopamine and epinephrine infusions simultaneously after giving atropine? Or is it an either/or decision?
Jeff with admin. says
It is an either/or decision. You will administer either dopamine or epinephrine.
Kind regards,
Jeff
Kelly Buford says
Thanks! Really appreciate this website! Worth every cent.