Early Identification and EMS Activation
Early identification of stroke symptoms in the out-of-hospital setting is critical for improved outcomes. Every year nearly 800,000 people suffer from a stroke. Eighty-seven percent of these strokes are ischemic and if caught early could potentially be treated with fibrinolytic therapy.
Since the goal of stroke therapy is to minimize brain injury and maximize recovery, early recognition of acute ischemic stroke and activation of EMS is the first step in the stroke algorithm.
Signs and symptoms of stroke include rapid onset of any of the following symptoms: weakness or numbness which will most likely be limited to one side of the body, confusion, trouble walking, loss of vision in one or both eyes, difficulty with speech or comprehension, severe headache with no known cause, and/or loss of balance and coordination.
Prehospital emergency services
Health care providers should be familiar with the Cincinnati Prehospital Stroke Scale. This simple scale is used to rapidly assess a patient for possible stroke.
Cincinnati Prehospital Stroke Scale:
The Cincinnati Prehospital Stroke Scale (CPSS) is used as an out-of-hospital assessment tool to help determine the neurologic status and ensure RAPID RECOGNITION of a stroke.
The CPSS uses three physical findings to determine the presence of stroke and if any one of these findings are present, stroke should be suspected and treated accordingly.
These three physical findings are:
1. Facial Droop; 2. Arm drift; 3. Abnormal speech.
Facial Droop is tested by having the patient smile and show their teeth. If the smile is asymmetrical or does not move the same as the other side this would be considered abnormal.
Arm drift is tested by having the patient close their eyes and extend both arms straight out in front of their body with the palms up for 10 seconds. If one arm does not move the same as the other one or if one arm drifts down compared to the other one, this would be considered abnormal.
Abnormal speech is tested by having the patient say “you can’t teach an old dog new tricks.” If the patient slurs words, uses incorrect words, or is unable to speak, this would be considered abnormal.
When providers are trained to use the CPSS they were able to recognize 86 to 97% of stroke patients as compared to 61-66% that were recognized prior to the CPSS training.
An important point of emphasis for Step #1 is that early notification to the receiving hospital of a potential stroke victim improves the speed with which they are treated after arrival at the emergency department.
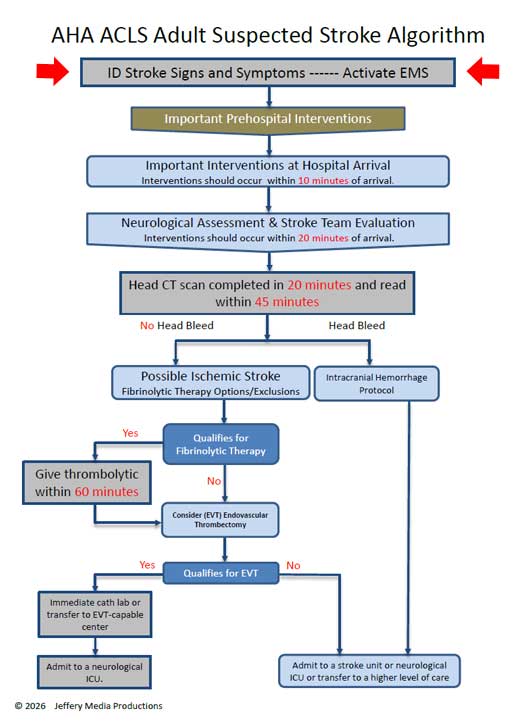
Rapid treatment for suspected stroke includes timing guidelines that have been incorporated into the AHA ACLS Suspected Stroke Algorithm. In the stroke algorithm diagram, the timing guidelines are highlighted in RED.
tpreidtp says
Hey Jeff,
I love this site! I use it every time I need to recertify.
It’s easy for me to choose a correct answer out of multiple choice, but that kind of training doesn’t translate well to the real world for me. The megacode videos are wonderful and the best way for me to learn and review. I would love to see the same type of videos for adult stroke. Will that be coming anytime soon? Please consider it!
Thanks for all you do and keep up the great work.
ACLS says
I would definitely love to get something like that added. I will add that to my list of things to work on for sure. Thank you so much for the suggestion. Kind regards, Jeff
Elaine McKinney says
I agree on all comments. great algorithm
LouiseAW says
We dont use the old FAST ? …no time element ?
cancelm5 says
so… for all strokes suspected patients this Cincinnati scale is used by the ems personnel prior to hospital arrival? Very nice and well explained. Thank you
Maria C.
Jeff with admin. says
Yes, the Cincinnati stroke scale is typically the scale used for rapid and early recognition of suspected stroke in the out of hospital setting. Kind regards, Jeff
Shanda Thrush says
Very easy to understand so that even the lay person could perform the above assessment.
M.M. says
When compared with the standard manual this single page is more clear and comes to the point.
Great!
Ita Sunday says
Impressive. Thanks for a job welldone
Nancy says
This is clear and concise..I just love how you simplified the process in an orderly concise way!