 The Cardiac Arrest Algorithm takes its place as the most important algorithm in the ACLS Protocol. There are 4 rhythms that are seen with pulseless cardiac arrest. They each will be reviewed throughout this section of the course guide. These four rhythms are pulseless ventricular tachycardia (VT), ventricular fibrillation (VF), asystole, and pulseless electrical activity (PEA).
The Cardiac Arrest Algorithm takes its place as the most important algorithm in the ACLS Protocol. There are 4 rhythms that are seen with pulseless cardiac arrest. They each will be reviewed throughout this section of the course guide. These four rhythms are pulseless ventricular tachycardia (VT), ventricular fibrillation (VF), asystole, and pulseless electrical activity (PEA).
Click below to view the cardiac arrest algorithm diagram. When done click again to close the diagram.
Cardiac Arrest Diagram
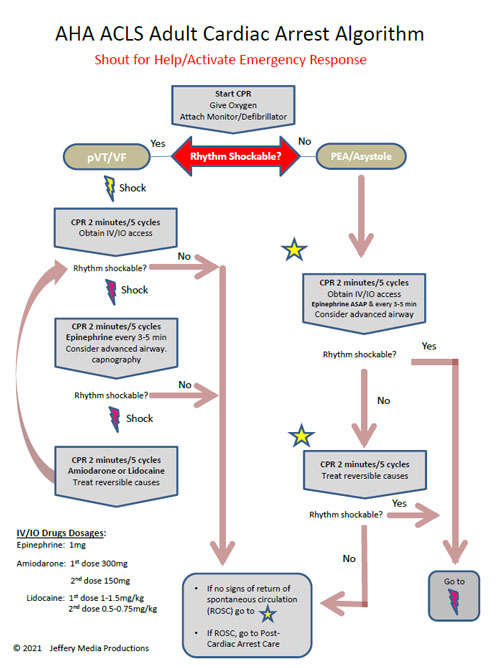
The majority of patients that experience sudden cardiac arrest will be treated with the Cardiac Arrest Algorithm. Therefore, mastery of this algorithm is very important. There are 2 branches of the Cardiac Arrest Algorithm, the left, and right branch.
The LEFT BRANCH is used for the treatment of pulseless ventricular tachycardia and ventricular fibrillation,and the RIGHT BRANCH is used for the treatment of PEA and Asystole.
Medications for Cardiac Arrest
There are 3 medications that will be focused on within the Cardiac Arrest Algorithm, epinephrine, amiodarone, and Lidocaine. Magnesium will be mentioned briefly.
Epinephrine
Epinephrine is the primary drug used in the cardiac arrest algorithm. It is used for its potent vasoconstrictive effects and also for its ability to increase cardiac output. Epinephrine is considered a vasopressor.

Indications for Cardiac Arrest
- Vasoconstriction effects: epinephrine binds directly to alpha-1 adrenergic receptors of the blood vessels (arteries and veins) causing direct vasoconstriction, thus, improving perfusion pressure to the brain and heart.
- Cardiac Output: epinephrine also binds to beta-1-adrenergic receptors of the heart. This indirectly improves cardiac output by:
- Increasing heart rate
- Increasing heart muscle contractility
- Increasing conductivity through the AV node
Routes
During ACLS, epinephrine can be given 3 ways: intravenous; intraosseous, and endotracheal tube. The primary method used is intravenous. When given intravenously, always follow the IV push with a 20 ml normal saline flush.
Dosing
Intravenous Push/IO: 1mg epinephrine IV is given every 3-5 minutes.
Note: There is no clinical evidence that the use of epinephrine when used during cardiac arrest, increases rates of survival to discharge from the hospital. However, studies have shown that epinephrine and vasopressin improve rates of ROSC (return of spontaneous circulation).
Amiodarone
Indications for ACLS
Amiodarone is an antiarrhythmic that is used to treat both supraventricular arrhythmias and ventricular arrhythmias.
The mechanism of action of amiodarone remains unknown, but within the framework of ACLS, amiodarone is used primarily to treat ventricular fibrillation and ventricular tachycardia that occurs during cardiac arrest and is unresponsive to shock delivery, CPR, and vasopressors.
Amiodarone should only be used after defibrillation/cardioversion and epinephrine have failed to convert VT/VF.
Route
Amiodarone can be administered by intravenous or intraosseous route.
Dosing
The maximum cumulative dose in a 24 hour period should not exceed 2.2 grams.
Within the VT/VF pulseless arrest algorithm, the dosing is as follows:
300mg IV/IO push → (if no conversion) 150 mg IV/IO push → (after conversion) Infusion #1 360 mg IV over 6 hours (1mg/min) → Infusion #2 540 mg IV over 18 hours (0.5mg/min)
Infusions exceeding 2 hours must be administered in glass or polyolefin bottles containing D5W.
Amiodarone should only be diluted with D5W and given with an in-line filter.
Lidocaine
Lidocaine is an antiarrhythmic that can also be used and is considered equivalent to amiodarone in the treatment of ventricular fibrillation or pulseless ventricular tachycardia.
Dosing
Provide an initial dose of 1-1.5 mg/kg IV or IO. If pVT or VF persists the lidocaine may be repeated at 0.5-0.75 mg/kg over 5 to 10 minute intervals.
The maximum total dosage of lidocaine is 3 mg/kg.
Magnesium Sulfate
Magnesium sulfate can be used during cardiac arrest primaryly to treat torsades de pointes that is caused by a low serum magnesium level.
Dosing
Provide an initial dose of 1-2 grams IV or IO diluted in at least 10 ml of NS. Give the dose over 5 minutes.
Watch Part 1 and Part 2 of the Cardiac Arrest Video Review.
Within ACLS Protocol, there is also a Simplified Cardiac Arrest Algorithm that simplifies and streamlines uncomplicated cardiac arrest. Use this link to watch a short video that reviews the 2015 Simplified Cardiac Arrest Algorithm.
Top Questions Asked on This Page
-
Q: Can precordial thump still be used for witnessed arrest?
A: This is the AHA position and it has not changed since 2010. “The precordial thump may be considered for termination of witnessed monitored unstable ventricular tachyarrhythmias when a defibrillator is no immediately ready for use, but should not delay CPR and shock delivery. There is insufficient evidence to recommend for or against the use of the precordial thump for witnessed onset of asystole.
-
Q: How fast do you push the Amiodarone 300mg?
A: In a cardiac emergency, you will push amiodarone as fast as you can push the plunder of the syringe. Essentially the same as you would push any drug in a cardiac emergency.
-
Q: I keep getting confused about when to return to administration of epinephrine following the initial dose and admin of 300/150 amiodarone…is it based on time (q 3-5 min)? Any suggestions on how to keep this straight?
A: After the first dose of epinephrine, it is essentially on its own time table. Just remember to give epinephrine every 3-5 minutes after the first dose. Amiodarone is given after the 3rd (300mg) shock and any time after 4th (150mg) shock.
-
Q: If you give precordial thump, is it given just once?
A: Yes, the precordial thump is attempted only one time. it is effective only if used near the onset of VF or pulseless VT, and so should be used only when the arrest is witnessed or monitored and only at the outset. . About 25% of patients in cardiac arrest who received a thump on the precordium regained cardiac function according to one study. There is no evidence that the precordial thump improves recovery in unwitnessed cardiac arrest.
Will says
I am wondering what evidence there is to support 20 mL flushes. I have not seen any specific volumes for flushes in the AHA algorithm and I have only seen 10 mL flushes in practice. Are we losing efficacy by flushing with 10 mL or are we losing time by using two 10 mL flushes?
ACLS says
The 2020 AHA guidelines specify a 20 mL saline flush after IV epinephrine during cardiac arrest to ensure drug delivery.
Here’s the exact quote with the reference:
“Each dose given by peripheral injection should be followed by a 20-mL flush of IV fluid to ensure delivery of the drug into the central compartment.” Reference
Kind regards,
Jeff
Tracey says
If you have to push Amiodarone IV what do you mix it with in a 10ml syringe? I know if you infuse it through the IV pump it needs to be mixed with a bag of D5W, but what if you have to fast push it; then what do you mix it with? Do you still spike a D5W bag and pull out what you need, and how much of that do you pull out in a syringe to give the amiodarone?
ACLS says
In an emergency situation where rapid administration of amiodarone is required, the following guidelines apply:
Emergency IV Push Administration of Amiodarone
For rapid IV push administration, amiodarone can be given undiluted or minimally diluted.
If dilution is preferred, use D5W (5% Dextrose in Water) to dilute amiodarone.
You can administer this undiluted, or dilute it with 4 mL of D5W to make a total volume of 10 mL (300 mg/10 mL)
Administer the dose rapidly over 1-3 minutes.
Follow the amiodarone push with a 20 mL normal saline flush.
Important Notes
Normal saline (NS) should not be used to dilute amiodarone due to potential precipitation, but it can be used as a flush after administration.
Rashhh says
Hi! I’m a little bit confused with how the Epinephrine and Amiodarone works in timing. Correct me if I’m wrong.
Initiate CPR; FIRST rhythm check > PEA/ASY > will give epinephrine.
If the FIRST rhythm check is pVT/VF, shock the patient. If after the SECOND rhythm check is pVT/VF, we will give Epinephrine. After THIRD shock, if it is still pVT/VF, Amiodarone 300 mg should be given. Will I wait for another 3-5 minutes for the Epinephrine to be given AFTER the Amiodarone or just continue to give the Epi after 3-5 minutes from the first dose?
7:30 START CPR
7:32 pVT/VF ->>> 1ST SHOCK, CONTINUE CPR
7:34 pVT/VF ->>> 2ND SHOCK + FIRST EPINEPHRINE while continuing CPR
7:36 pVT/VF ->>> 3RD SHOCK + 300 MG AMIODARONE while continuing CPR
7:38 pVT/VF ->>> 4TH SHOCK + 150 MG AMIODARONE while continuing CPR
Will I give the Epinephrine around 7:37 to 7:39? Because that’s the 3-5 minutes window for the Epinephrine.
Or will I wait another 3 minutes after the FIRST Amiodarone was given.
Please correct my timeline. I would love to hear from you. Thank you so much!
ACLS says
You are correct in saying that the epinephrine is first given after the second shock during CPR. After the first dose of epinephrine is administered, epinephrine is on its own timetable, and is given every 3 to 5 minutes regardless of everything else that is going on.
Amiodarone 300 mg is given first after the third shock during CPR. The second bolus of amiodarone may be given after the 4the shock if it is needed for refractory VF or pVT.
Kind regards,
Jeff
Lisa Chan says
Hello, I have 2 questions:
1) According to cardiac arrest algorithm, if a non-shockable rhythm converts to a shockable rhythm during rhythm shock, then we will follow the VF/ pVT pathway. Is it true that we can give enpinephrine/ amiodarone already after 1st shock (rather than give epinephrine after 2nd, give amiodarone after 3rd shock if we go over the VF/ pVT algorithm from the beginning)? If yes, how do we decide if we give epinephrine/ amiodarone first?
2) Can you clarify if the dosage of MgSO4 for torsades de pointes is different for cardiac arrest and torsades de pointes with pulse? If yes, what are the dosages for each scenario?
Thank you so much!
ACLS says
1. This would be at the discretion of the physician that is leading the code. If the first dose of epinephrine was given when following the asystole/pea branch then it’s likely that a physician would carry on at the second administration of epi which would put the dose given after the first shock and the amiodarone given after the 2nd shock.
2. Dosage is the same. The recommended initial dose of magnesium is a slow 2 g IV push. An infusion of 1 gm to 4 gm/hr should be started to keep the magnesium levels greater than 2 mmol/L. Once the magnesium level is greater than 3 mmol/L, the infusion can be stopped
Kind regards,
Jeff
RJ says
For Amiodarone administration, is it after 3 shocks in a row? Or 3 shocks intermittently at anytime? Or both?
Example: I get vfib and shock, then it goes into PEA, then vfib two more times. Would I shock even though it wasnt three in a row?
ACLS says
Amiodarone administration in cardiac arrest is typically recommended after 3 shocks for persistent or recurrent ventricular fibrillation (VF) or pulseless ventricular tachycardia (pVT), regardless of whether these shocks occur consecutively or intermittently.
In your example scenario:
Initial VF – shock given
PEA (no shock)
VF – shock given
VF – shock given
After this third shock for VF, even though it wasn’t three consecutive shocks, amiodarone would be indicated if the VF/pVT persists.
The key points regarding amiodarone administration in cardiac arrest are:
It is given for shock-refractory VF/pVT, defined as VF/pVT that persists or recurs after one or more defibrillation attempts.
The initial dose is 300 mg IV/IO push after the third shock.
A second dose of 150 mg can be considered after the fifth shock if VF/pVT persists.
Amiodarone is given in conjunction with high-quality CPR, defibrillation attempts, and epinephrine administration as indicated by the cardiac arrest algorithm.
Simona Dumitru says
Do you stop CPR for advanced airway, endotracheal tube for exemple? Thank you. ( As usual, like years before, super informed and very good structured informations. Thanks again for your admirable work!)
ACLS says
Brief cessation of CPR is usually necessary for placement of an endotracheal tube.
Kind regards,
Jeff
Tera Messner says
Is there a place within your site that I can click on the various algorithms to print for studying purposes? Please let me know. Thanks.
Tera
ACLS says
You can download algorithm printouts in the download library.
Kind regards,
Jeff
connie says
So say you gave after fourth shock -150mg amiodarone- and after another cycle of cpr you have administered epi after 5th shock. but now 6th shock comes around do you still give 150 mg amiodarone or is the dose higher or even less than this? Or will you start to infuse the drug after the of 150 mg amiodarone and your coming up to a time when you want to give it again?
ACLS says
During cardiac arrest, the first dose of amiodarone IV push is 300 mg. The second dose would be 150 mg. These two doses are the only doses that are given during cardiac arrest. If cardiac arrest continues to be refractory in spite of all efforts up to this point it is unlikely that giving more amiodarone will reverse the problem. If the patient does experience ROSC and tachyarrhythmias persist then and amiodarone infusion would be started.
Kind regards,
Jeff
Zhilam Zia says
I like to thank you very much for nice clarification about treatment of VF. Would you please let me know about any role of IV amiodarone in hemodynamically unstable VT with pulse if Synchronized DC shock can not be given due to any reason ?
Secondly, which one is best in Stable VT with pulse, IV amiodarone or procainamide ? Thanks and best regards.
ACLS says
Amiodarone is the first recommended antiarrhythmic for the treatment of stable and unstable VT. There are no major reasons for withholding amiodarone unless there has been a previous negative reaction with the medication.
I personally have not seen procainamide used in years so I cannot speak specifically about it use. Amiodarone is the antiarrhythmic of choice.
Kind regards,
Jeff
Elizabeth Owens says
I was wondering why the dosing interval is every 3-5 minutes other than that’s what the ACLS says?
Jeff with admin. says
Since the half-life of epinephrine is 5-10 minutes you give the epinephrine every 3-5 minutes. This keeps the epinephrine at peak levels. Giving it outside of the 3-5 minute parameter allows the epinephrine levels in the blood to be either higher than needed or lower that needed. Kind regards, Jeff
Christopher P Kenner says
If epi was administered initially via IO, a second dose was 7 minutes later, and a third was also given at 7 minutes, what if any, contraindications would thete be?
ACLS says
There would not be any contraindication, however, the epinephrine half-life is two minutes. Therefore, there would be a great potential for the blood levels of epinephrine would drop to low between the doses. This is why epinephrine doses are set to be given every 3–5 min.
Kind regards,
Jeff