
Often cardiac arrest in children is associated with a reversible condition or cause, and identification of reversible causes of pediatric cardiac arrest is critical for its successful treatment.
Since sudden cardiac arrest is not typical in the pediatric population, there will likely be progressive signs and symptoms before the arrest which can help you identify reversible causes. Ensure that you obtain a reasonable physical assessment and history of illness. The physical assessment and history of illness will help direct your management and lead to optimum treatment with positive outcomes.
The reversible causes and contributing factors can be summarized using the mnemonic of the PALS H’s and T’s.
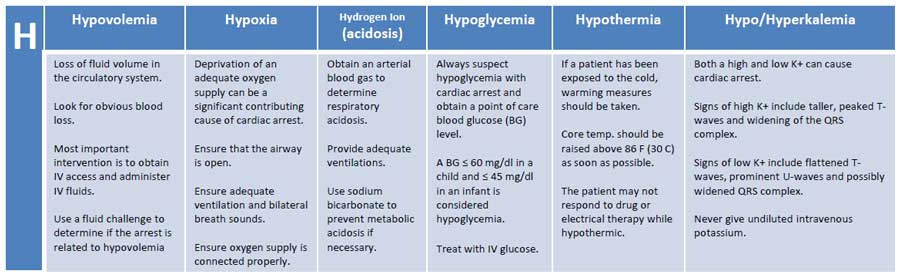
(Download PALS H’s and T’s Cheat Sheet)
Hypovolemia:
Hypovolemia, the loss of fluid volume in the circulatory system, can be a major contributing cause to cardiac arrest.
Looking for obvious blood loss in the patient with pulseless arrest is the first step in determining if the arrest is related to hypovolemia. After CPR, the most important intervention is obtaining intravenous access/IO access. A fluid challenge (fluid bolus) may also help determine if the arrest is related to hypovolemia.
(See also Hypovolemic Shock Page.)
Hypoxia:
Hypoxia, deprivation of adequate oxygen supply, can be a significant contributing cause to cardiac arrest.
You must ensure that the patient’s airway is open and that the patient has chest rise and fall and bilateral breath sounds with ventilation. Also, ensure that your oxygen source is connected properly. (See Respiratory Distress/Failure Page)
Hydrogen Ion (Acidosis):
To determine if the patient has respiratory acidosis, an arterial blood gas evaluation must be performed. Prevent and treat respiratory acidosis by providing adequate ventilation. Prevent metabolic acidosis by giving the patient sodium bicarbonate.
Hyper/Hypokalemia:
Both a high potassium level and a low potassium level can contribute to cardiac arrest. The major sign of hyperkalemia, high serum potassium, is taller and peaked T-waves. Also, a widening of the QRS-wave may be seen. This can be treated with a variety of interventions which include sodium bicarbonate (IV), glucose+insulin, calcium chloride (IV), Kayexalate, dialysis, and possibly albuterol. All of these will help reduce serum potassium levels.(See Hyperkalemia and Cardiac Arrest Page)
The major signs of hypokalemia, low serum potassium, are flattened T-waves, prominent U-waves, and possibly a widened QRS complex. Treatment of hypokalemia involves rapid but controlled infusion of potassium. Giving IV potassium has risks. Always follow the appropriate infusion standards. Never give undiluted intravenous potassium.
Hypoglycemia:
Hypoglycemia, low serum blood glucose, can have many negative effects on the body and it is a common finding among critically ill children. Normal blood glucose levels should be greater than 60 mg/dl in children and 45 mg/dl in infants.
Treat hypoglycemia with IV dextrose to reverse a low blood glucose.
Hypothermia:
If a patient has been exposed to the cold, warming measures should be taken. The hypothermic patient may be unresponsive to drug therapy and electrical therapy (defibrillation or pacing) until warmed. Core temperature should be raised above 86 F (30 C) as soon as possible.
(Download PALS H’s and T’s Cheat Sheet)
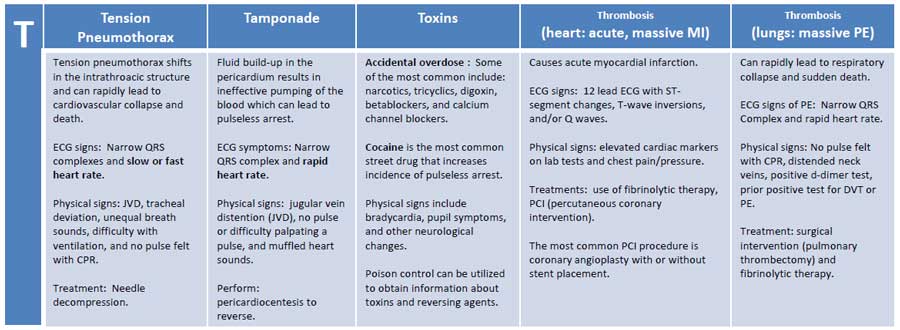
Tension Pneumothorax:
Tension pneumothorax occurs when air is allowed to enter the pleural space and is prevented from escaping naturally. This leads to a build-up of tension that causes shifts in the intrathoracic structure that can rapidly lead to cardiovascular collapse and death. ECG signs include narrow QRS complexes and slow heart rate. Physical signs include JVD, tracheal deviation, unequal breath sounds, difficulty with ventilation, and/or no pulse felt with CPR. Treatment of tension pneumothorax is needle decompression. (See Obstructive Shock Page)
Tamponade:
Cardiac tamponade is an emergency condition in which fluid accumulates in the pericardium (sac in which the heart is enclosed). The build-up of fluid results in the ineffective pumping of the blood which can lead to cardiac arrest. ECG symptoms include narrow QRS complex and rapid heart rate. Physical signs include jugular vein distention (JVD), no pulse or difficulty palpating a pulse, and muffled heart sounds due to the fluid inside the pericardium. The recommended treatment for cardiac tamponade is pericardiocentesis. (See Obstructive Shock Page)
Toxins:
Accidental overdose of several different kinds of medications can cause pulseless arrest. The arrest may be a result of direct cardiac toxicity or the secondary effects of respiratory depression or circulatory side effects.
Ensure rapid communication with a poison control center. (1-800-222-1222)
Some of the most common toxins include those that cause respiratory depression resulting in cardiac arrest. Examples include opioids, benzodiazepines, and ETOH. The focus of support for cardiac arrest caused by this type of toxin should focus on support of airway and ventilations and administration of antidotes when indicated. (See Disordered Control of Breathing Page)
Reversing agent for opioids: Naloxone
Reversing agent for benzodiazepines: Romazicon
Some other medications can become toxic and increase the risk of the development of Torsades de Pointes (polymorphic VT). These include antiarrhythmics such as amiodarone and sotalol, tricyclic antidepressants, and calcium channel blockers.
Medication overdose or toxicity may also increase the risk of bradyarrhythmias. Medications to consider when bradyarrhythmias are present include calcium channel blockers, Beta-adrenergic blockers, digoxin, opioids, clonidine, cholinesterase inhibitors, and succinylcholine.
Support of circulation while an antidote or reversing agent is obtained is of primary importance. Poison control can be utilized to obtain information about toxins and reversing agents.
Frequently, toxicity is temporary, and prolonged resuscitation efforts may be necessary. This prolonged effort may significantly improve long-term survival, and ECMO (extracorporeal membrane oxygenation) may also significantly improve long-term survival while toxins are given the time to be reversed or metabolized.
Thrombosis (heart: acute, massive MI):
Although rare in infants and children, coronary thrombosis is an occlusion or blockage of blood flow within a coronary artery caused by blood that has clotted within the vessel. The clotted blood causes an acute myocardial infarction which destroys heart muscle and can lead to sudden death, depending on the location of the blockage.
ECG signs during PEA indicating coronary thrombosis include ST-segment changes, T-wave inversions, and/or Q waves. Physical signs include elevated cardiac markers on lab tests.
Thrombosis (lungs: massive pulmonary embolism):
Pulmonary thrombus or pulmonary embolism (PE), which is also rare in children, is a blockage of the main artery of the lung, which can rapidly lead to respiratory collapse and sudden death.
There are some causes that should be considered when evaluating for pulmonary embolism. Embolism can be caused by a blood clot, catheter fragment, fat, air, or injected foreign material.
There are some factors which predispose certain populations of children to intravascular thrombosis. These include sickle cell disease, malignancy, coagulation disorders, and the presence of an indwelling central venous catheter.
Identification of PE may be difficult in children because the signs are very subtle and nonspecific. ECG signs of PE include narrow QRS Complex and rapid heart rate. Physical signs include no pulse felt with CPR, distended neck veins, positive d-dimer test, and/or prior positive test for DVT or PE. Treatment includes surgical intervention (pulmonary thrombectomy) and fibrinolytic therapy.
(See PALS Obstructive Shock Page for recognition and management details)
Trauma
Although not specifically included in the PALS H’s and T’s, cardiac arrest caused by unrecognized trauma is something that should be given consideration.
Trauma can be a cause of pulseless arrest, and a proper evaluation of the patient’s physical condition and history should reveal any traumatic injuries. Treat each traumatic injury as needed to correct any reversible cause or contributing factor to the pulseless arrest.
Part 4: Management of Cardiac Arrest and Cardiac Arrest Algorithm
Dr Abdullahi says
This is an interesting publication and easy to understand by a medical practitioner
Terry Hollowell says
Your site is just great. Been studying for about an hour per day as a refresher for upcoming courses. Maybe consider taking out apostrophe on H’s and T’s as it should read correctly as Hs and Ts (known as grocer’s apostrophe, a common mistake) as they do not have “ownership”. Any rate, thanks for all the great advise.
Terry
ACLS says
Thanks so much for the encouraging words and thank you for pointing out the apostrophe issue. I will try to get that taken care of. Kind regards, Jeff