 Tachycardia/tachyarrhythmia is defined as a rhythm with a heart rate greater than 100 bpm.
Tachycardia/tachyarrhythmia is defined as a rhythm with a heart rate greater than 100 bpm.
An unstable tachycardia exists when cardiac output is reduced to the point of causing serious signs and symptoms.
Serious signs and symptoms commonly seen with unstable tachycardia are: chest pain, signs of shock, SOA (short of air), altered mental status, weakness, fatigue, and syncope.
One important question you may want to ask is: “Are the symptoms being caused by the tachycardia?” If the symptoms are being caused by the tachycardia treat the tachycardia.
Causes
There are many causes of both stable and unstable tachycardia and appropriate treatment within the ACLS framework requires identification of causative factors. Before initiating invasive interventions, reversible causes should be identified and treated.
The most common causes of tachycardia that should be treated outside of the ACLS tachycardia algorithm are dehydration, hypoxia, fever, and sepsis. There may be other contributing causes and a review of the H’s and T’s of ACLS should take place as needed.
Click below to view the H and T’s table. When done click again to close the diagram.
H’s and T’s Table
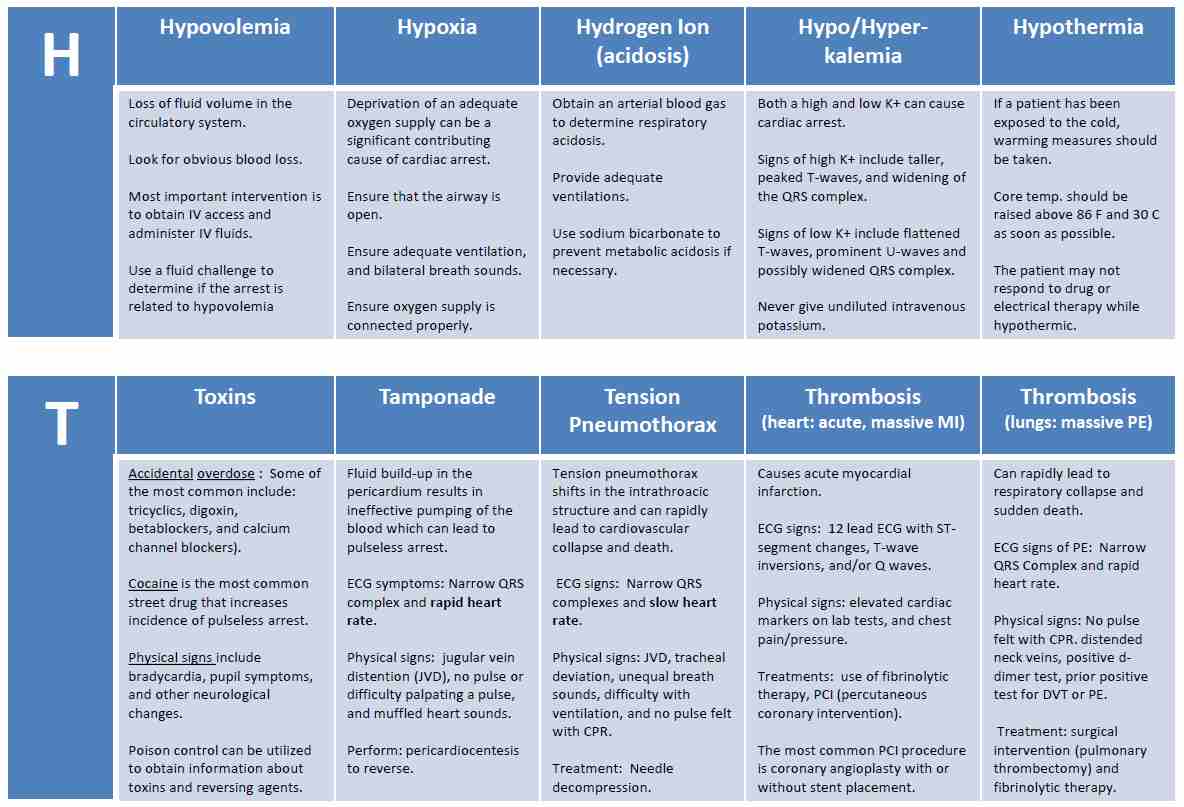
Administration of OXYGEN and NORMAL SALINE are of primary importance for the treatment of causative factors of sinus tachycardia and should be considered prior to ACLS intervention.
Once these causative factors have been ruled out or treated, invasive treatment using the ACLS tachycardia algorithm should be implemented.
Associated Rhythms
There are several rhythms that are frequently associated with stable and unstable tachycardia these rhythms include:
- Supraventricular tachycardia (SVT)
- Atrial fibrillation
- Atrial flutter
- Monomorphic VT
- Polymorphic VT
- Wide-complex tachycardia of uncertain type
ACLS Treatment for Tachycardia
Click below to view the tachycardia algorithm diagram. When done click again to close the diagram.
Tachycardia Diagram
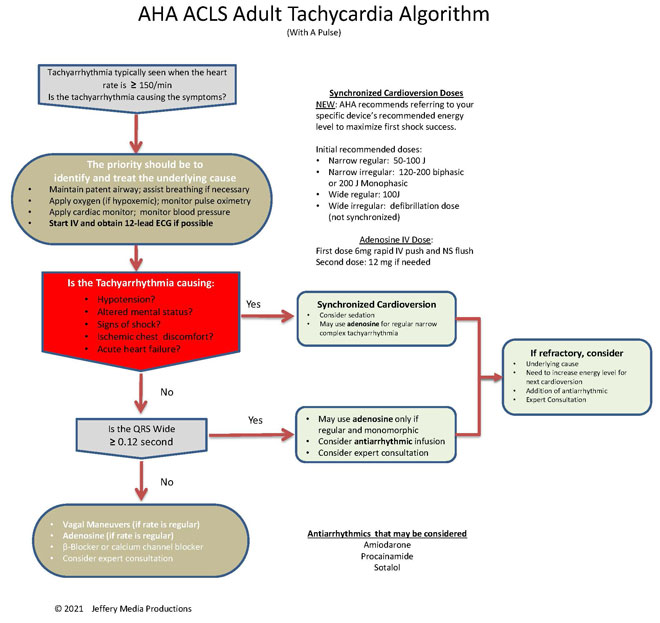
or Members Download the Hi-Resolution PDF Here(This will open in another window.)
The first question that should be asked when initiating the ACLS tachycardia algorithm is: “Is the patient stable or unstable?” The answer to this question will determine which path of the tachycardia algorithm is executed.
Unstable Tachycardia
Patients with unstable tachycardia should be treated immediately with synchronized cardioversion. If a pulseless tachycardia is present patients should be treated using the cardiac arrest algorithm.
The AHA no longer provides specific shock dose recommendations for synchronized cardioversion. Instead, they instruct to refer to your specific device’s recommended energy level to maximize first shock success.
For the purposes of a basic understanding of cardioversion, the information about general shock dosages and recommendations will remain in the content on this website.
The initial recommended synchronized cardioversion voltage doses are as follows:
- narrow regular: 50-100 J; i.e., SVT and atrial flutter
- Narrow irregular: 120-200 J biphasic or 200 J monophasic; i.e., atrial fibrillation
- Wide regular: 100 J; i.e., monomorphic VT
- Wide irregular: defibrillation dose (not synchronized)
Stable Tachycardia
Patients with stable tachycardia are treated based upon whether they have a narrow or wide QRS complex. The following flow diagram shows the treatment regimen for stable tachycardia with narrow and wide QRS complex.
- Stable (narrow QRS complex) → vagal maneuvers → adenosine (if regular) → beta-blocker/calcium channel blocker → get an expert
- Stable (wide/regular/monomorphic) → adenosine → consider antiarrhythmic infusion → get an expert
Lisa Chan says
Hello, may I ask at most doses of adenosine can we give for SVT, since some sources mention give 6mg adenosine for first dose, followed by 12mg adenosine for second dose if needed; whereas some sources mention can even consider giving another second dose 12mg for one more time (i.e. 3 doses in total). So, for your expert opinion, at most should we give 2 or 3 doses of adenosine before considering other medications (e.g. BB, CCB)? Thank you very much!
ACLS says
American heart association has two doses of adenosine listed, 6 mg and then 12 mg. In previous guidelines prior to 2015, there were three doses of adenosine listed in the algorithm 6mg, 12mg, 12mg. This third dose would be up to the physicians discretion and it can be done. The AHA provides guidelines for providers, and then the providers are ultimately responsible to strictly follow the guidelines or use their best clinical judgments to deviate when needed. I think that there may be times where a third dose of 12 mg is clinically indicated.
Kind regards,
Jeff
Cathy says
Hi
What to do with a stable patient with wide complex tachycardia with whom cardioversion with adenosine (6mg, then 12mg) has failed?
ACLS says
Some providers based upon their own clinical judgment, may attempt another 12 mg of adenosine. Expert consultation with a cardiologist would be the next step. There are a number of things that need to be considered, when addressing wide complex tachycardia and since the patient is stable, expert consultation would be advised.
Kind regards, Jeff
Sophia says
Hello Jeff,
I am reviewing the Tachycardia with a pulse algorithm and would like clarification.
Specifically, Unstable Tachycardia. When the patient is showing signs of instability with Tachycardia, we will cardiovert.
A. However, in Unstable, irregular and wide, we will Defibrillate if its Torsades, no dig,ccb or BB because that can block AV node pathway causing increase in ventricular response.
B. In Unstable, regular and wide, we will sync & cardiovert. If Refractory, we Increase energy level, look at underlying cause and get Expert consultation ( no antiarrythmics recommended as it may cause more harm)
C. if Unstable, irreg and narrow- 1. Do we cardiovert despite risk of clots? 2. There’s a contraindication with CCB and BB – how do we manage rate control with this group?
ACLS says
Hi Sophia,
Unstable tachycardia with an irregular rate and narrow QRS may be due to atrial fibrillation, which carries a risk of forming blood clots in the atria.
Therefore, before performing cardioversion, it is important to assess the patient’s risk of thromboembolism.
The risk of thromboembolism can be estimated using various scoring systems, such as the CHADS2 or CHA2DS2-VASc score. These scores take into account factors such as age, gender, history of stroke or transient ischemic attack, hypertension, diabetes, and congestive heart failure.
If the patient has a high risk of thromboembolism, anticoagulation therapy should be initiated before cardioversion.
In some cases, such as in unstable tachycardia with hemodynamic compromise, immediate cardioversion may be necessary even without anticoagulation therapy. In such cases, the benefits of cardioversion may outweigh the risks of thromboembolism.
Ultimately, the decision to perform cardioversion should be based on a careful assessment of the patient’s individual risk-benefit profile, taking into account the potential risks and benefits of the procedure, as well as the patient’s overall clinical condition and comorbidities. This decision should be made in consultation with a qualified healthcare provider.
Kind regards,
Jeff
Abbie says
Hi,
If a patient had a syncopal episode in the community and then was seen in the emergency department and found to be in SVT, would this be classed as stable or unstable?
If the patient was conscious and had no evidence of cerebral hypoperfusion at the time of assessment, but had a history of a syncopal episode, how should this be managed?
Many thanks,
A
ACLS says
The question of whether the patient is stable or unstable would be determined at the time of the assessment and based upon the patient’s condition at the time of the assessment. In the emergency room if they had no evidence of cerebral hypo perfusion and no signs or symptoms of instability then they would be considered stable.
Kind regards,
Jeff
Khine Khine says
Hi, a case of a patient with DDD(R) pacemaker underlying tachy-brady arrhythmia who developed fast atrial fibrillation. ECG generated HR of 157bpm and a patient is hypotensive and BP machine cannot capture the actual reading. Patient remains conscious and asymptomatic (No signs of cerebral hypo perfusion and shock).
Is it considered stable AF or unstable AF?
What would be the treatment to intervene fast AF? IV anti-arrhythmic or DC synchronised cardioversion?
ACLS says
That would be a borderline stable/unstable issue. If the patient is conscious and asymptomatic then the best thing would be to determine what that blood pressure is. Also, is there a palpable pulse? Sometimes a pulse pressure tells you a lot about perfusion.
I think most physicians in this case would go with a IV anti-arrhythmic. Would begin anticoagulant therapy if not already going and perform a transesophageal echocardiogram in order to prepare for synchronized cardioversion.
Kind regards,
Jeff
Rose says
If you do one dose of adenosine, can you then deem them unstable and cardiovert? Or do you need to do both doses?
ACLS says
And unstable condition would be identified based upon the patient’s vital signs and also the assessment. If the patient is unstable then different interventions other than adenosine should be used. Kind regards, Jeff
Robbie D says
If after the first initial shock during Cardio version at 50j you do not cardiovert, when time frame do you initiate the next 100j….150j…..200j?
ACLS says
A minimum of 1 minute should elapse between successive shocks to minimize myocardial damage.
Kind regards, Jeff
Shaz says
Hi, if patient have normal blood pressure (130/89mmHg) and pulse rate of 180, but have cool and clammy peripheries, is it stable or unstable tachycardia?
ACLS says
If these are the only symptoms that the patient is experiencing then this would be considered stable tachycardia.
Kind regards,
Jeff