
The pulseless ventricular tachycardia rhythm is primarily identified by several criteria. First, the rate is usually greater than 180 beats per minute, and the rhythm generally has a very wide QRS complex.
Second, the patient will be pulseless. And third, the rhythm originates in the ventricles. This is in contrast to other types of tachycardias which have origination above the ventricular tissue (in the atria).
Not all ventricular tachycardias are pulseless, and therefore, pulselessness must be established prior to beginning an algorithm. This is accomplished simply by checking a carotid or femoral pulse.
Pulselessness with a tachyarrhythmia occurs because the ventricles are not effectively moving blood out of the heart and there is, therefore, no cardiac output. Many tachyarrhythmias of a rate >150 will deteriorate into pulselessness if timely treatment is not given.
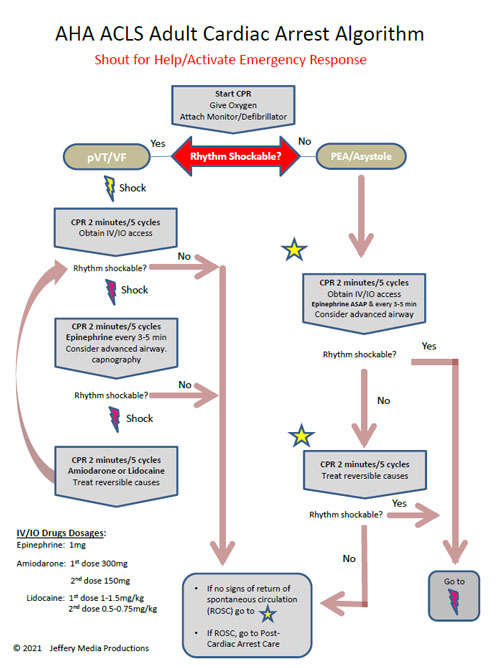
Pulseless ventricular tachycardia is treated using the left branch of the cardiac arrest algorithm. Click below to view the cardiac arrest algorithm diagram. When finished click again to close the diagram.
Cardiac Arrest Diagram
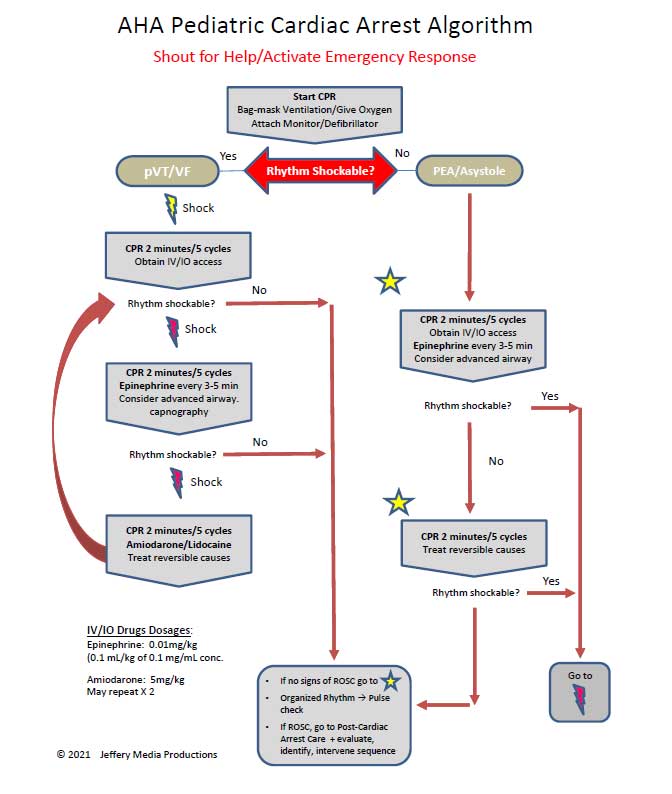
Click to view, and click again to close the diagram.
PALS Cardiac Arrest Diagram
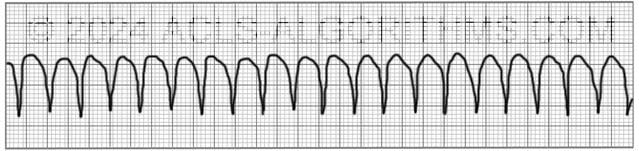
Play the video below to see what a Pulseless Ventricular Tachycardia will generally look like on a defibrillator monitor. Allow several seconds for video to load. (4.03 mb)
Click for next Rhythm Review: Ventricular Fibrillation
Top Questions Asked on This Page
-
Q: What happens after the 2nd dose of Amiodarone is given and the patient is still in the same rhythm? Do we give a 3rd dose immediately or rhythm usually changes after 2nd dose?
A: A 3rd and even a 4th dose of 150 mg amiodarone may be administered. The only thing that needs to be taken into consideration is the 2.2-gram maximum dosage for 24 hours. Also, it is unlikely that the rhythm will remain VF or pVT long enough for you to get to the 3rd or 4th dose.
-
Q: What does refractory VT or VF mean?
A: Refractory pVT or VF means that the VF or pVT does not convert to a perfusing rhythm and continues to persist in spite of multiple attempts at conversion with defibrilation, acls drugs, and high quality CPR.
-
Q: After initiating CPR and assessing the rhythm, the patient is in VF/ pVT and the first shock is given, and CPR for 2 mins. Then rhythm check and in VT, should the pulse be checked to confirm pVT?
A: If there is no rhythm change and the same waveform of VT continues, you would not need to perform a pulse check. Performing the pulse check would delay the continuation of chest compressions. Once VT is pulseless it is very unlikely that any VT will be able to produce life-sustaining cardiac contractions.
SUAN says
How do we identify pulseless VT/VF and PEA
Jeff with admin. says
You can review VT and VF here.
For PEA, if you have a patient that is unconscious with no pulse but they have a rhythm on the monitor that looks as if you should feel a pulse, you have PEA.
Kind regards,
Jeff
Phil says
I am a new nurse and currently working in the ICU . This is very helpfull and am hoping to pass my ACLS ( dunno when to take it yet just starting my own study). thanks:)
Grape123 says
Having trouble telling these apart – mono morphic v tach and pulse less v tach
Jeff with admin. says
The difference is not in the visual appearance. The difference is that one will have a pulse and the other will not. You can have monomorphic or polymorphic VT with or without a pulse.
Kind regards,
Jeff
Mylee Belle says
“Not all ventricular tachycardias are pulseless and therefore, pulselessness must be established prior to beginning an algorithm. This is accomplished simply by checking a carotid or femoral pulse.”
– for instances that all other criteria were present but not the pulselessness, (the patient has a palpable pulse) how do we proceed? thanks..your site is of great help..
Jeff with admin. says
You would proceed by using the tachycardia algorithm. You would first need to establish whether the patient is stable or unstable. This would dictate what your next step according to the tachycardia algorithm would be.
Kind regards,
Jeff
trwguitar says
This website is excellent! I have been a Registered Respiratory Therapist for 32 years, and I would personally recommend this website to anyone. It covers anything and everyhting you would need to prepare for acls. I’m very pleased, thank you!
Katrina Reyes says
why isn’t pulseless vtach treated like PEA in the acls algorithm?
Jeff with admin. says
There are two branches to the cardiac arrest algorithm. The right and left branch. The left branch is for treatment of Pulseless VT and VF and the right branch is for treatment of PEA/Asystole.
When a patient is in VT/VF, the shock (defibrillation) is used to temporarily stun the myocardial cells which will then “hopefully” reset to fire with the SA Node which is the pacemaker of the heart.
Shock (defibrillation) has been shown to be highly effective with the rhythms VT and VF. This is because there is an electrical current that is flowing in the heart and if these cells are stunned there is a good chance that they will reset to the firing of the SA node.
When you have a person who has PEA and asystole, there is no electrical current flow through the heart or at least not enough to be detected on the defibrillator/monitor. During this state it has been show that defibrillation does not produce any effective outcome.
Actually all of the interventions that are done in the right branch (PEA) are also carried out in the left branch (VT/VF) with the exception of adding shocks and a few other drugs which can be used for the treatment of the arrhythmia (VT/VF).
Kind regards, Jeff
Katrina Reyes says
This makes so much sense. I was always confused by the pulseless arrest algorithm because I thought pulseless VF and pulseless Vtach fit under the umbrella of PEA. Your website and customer service are excellent!
pennsyrn2006 says
Love this website! It helped me to do well on ACLS two years ago and I am recert-ing tomorrow! Thanks 🙂
DR Rafaqat ali says
very use full for acls
ANJALY ALIAS says
REALLY IT IS VERY USEFUL SITE FOR ACLS .THANK YOU VERY MUCH
Mitchfizzl says
I took my acls test the other day. This site was xtremly helpful. Thanks so much. I got a 90% on test.
Erin says
I’m taking my 2 day ACLS course tomorrow and this site is helping me make it through the pre-test. Thanks!
mariap says
Been on this site about one hour and already learning a lot. thanks!
mmarrujo says
Thank you…very helpful.
albert hanson says
Very good site and easy to understand.
Flotilde Samin says
Very simple explanation and organized easy to comprehend.