
Introduction:
Once ROSC is obtained, treatment moves from the cardiac arrest algorithm to the evaluate, identify, intervene sequence of the systematic approach algorithm.
During the post-cardiac arrest phase, a systems approach is used to support and maintain the stability of the patient.
The objective is to reduce morbidity and mortality through the assessment and management of the respiratory system, the cardiovascular system, and the neurologic system.
Each system is assessed and managed to ensure optimization of oxygenation, ventilation, and perfusion. These actions are carried out in order to stabilize cardiopulmonary function and preserve neurologic function.
Open the systematic approach algorithm diagram to visualize this movement from the cardiac arrest algorithm to the systematic approach algorithm.
Systematic Approach Diagram
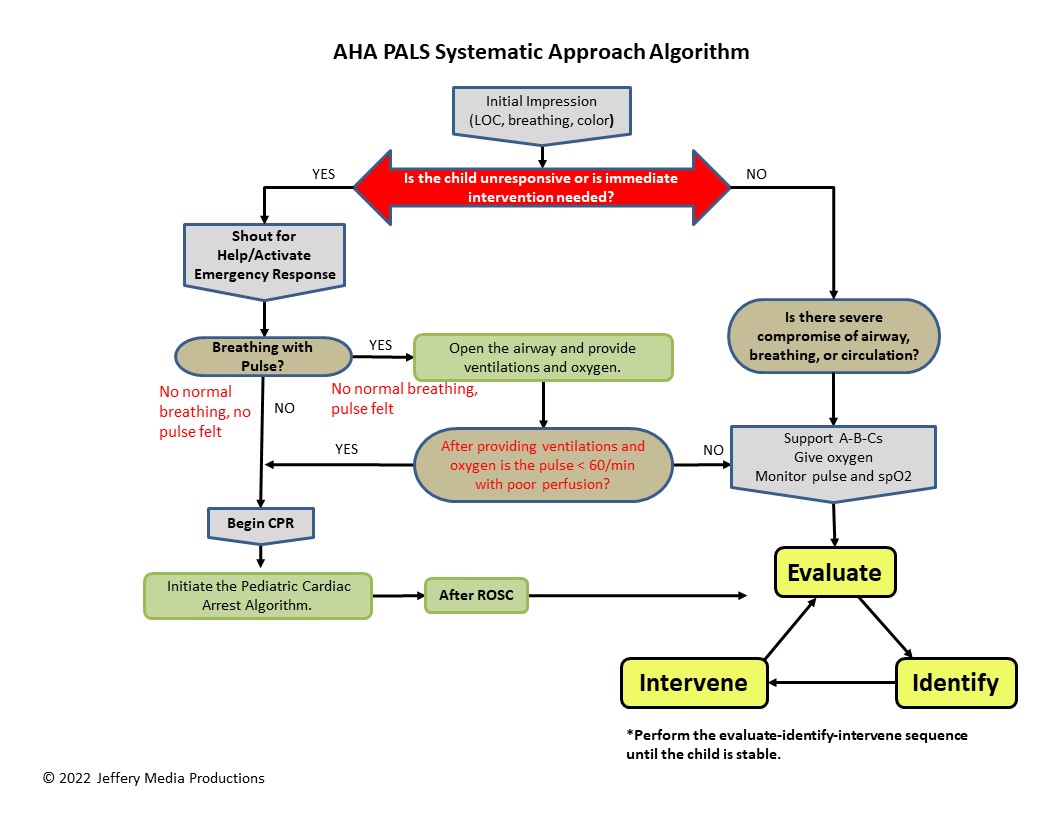
or Members Download the Hi-Resolution PDF here.
Goals for Post-Cardiac Arrest:
The goals for the post cardiac arrest phase center around the identification and treatment of organ system dysfunction.
Respiratory system:
- Optimize and stabilize airway, oxygenation, and ventilation
- Confirm proper ET tube placement
- Provide adequate oxygenation and ventilation
- Monitor end-tidal CO2 (Capnography), evaluate blood gas, chest x-ray
Goals:
Interventions:
Assessments:
Full Review: Respiratory System and Post Cardiac Arrest
Cardiovascular system:
- Support tissue perfusion and cardiovascular function
- Prevent shock
- Maintain adequate blood pressure and perfusion
- Treat arrhythmias
- Assess tissue perfusion by monitoring lactate concentration, venous oxygen saturation, and base deficit
- Hemodynamic monitoring of intra-arterial blood pressure
- Urine output, capillary refill, skin temperature
Goals:
Interventions:
Assessments:
Full Review: Cardiovascular System and Post Cardiac Arrest
Review of Post-Cardiac Arrest Shock
Review of Post-Cardiac Arrest IV Medications
Neurologic system:
- Neurologically intact survival
- Implement TTM (targeted temperature management)
- Avoid hyperthermia
- Adequate analgesia and sedation
- Treat seizures and increased intracranial pressure
- Avoid hyperventilation
- Monitor core temperature
- Point of care blood glucose level
- Perform ongoing neurological assessments