
Two types of bradycardia:
Primary bradycardia:
Primary bradycardia results from congenital abnormalities or acquired injury to the heart’s pacemaker cells or conduction system.
Some of the causes of primary bradycardia are myocarditis, surgical injury, cardiomyopathy, and congenital abnormalities of the heart or the heart’s conduction system.
Secondary bradycardia:
Non-cardiac problems cause secondary bradycardia. These problems result in abnormal functioning of the heart. Secondary bradycardia is typically the type of bradycardia seen in infants and children.
Non-cardiac problems that are the main cause of secondary bradycardia include hypoxia, acidosis, hypotension, hypothermia, and medication/drug side effects.
Evaluate:
Unlike bradycardia in adults, bradycardia due to a primary cardiac condition (primary bradycardia) is rare in children.
Pediatric bradycardia is defined as a heart rate that is below the normal heart rate range for the child’s age, level of activity, and clinical condition.
General Guide for Pediatric Bradycardia:
- 0-3 years old: HR < 100 bpm
- 3-9 years old: HR < 60 bpm
- 9-16 years old: HR < 50 bpm
Typically, symptomatic bradycardia is an ominous sign in infants and children, and it will be accompanied by hypotension, decreased level of consciousness, and signs of shock.
Symptomatic bradycardia is often seen before cardiac arrest and will also be accompanied by other signs of instability. Once it is recognized, it should be aggressively treated. The pediatric bradycardia algorithm helps to streamline and simplify the aggressive treatment that is needed.
Identify:
Once symptomatic bradycardia is recognized during the evaluation of a critically ill or injured child, seek to IDENTIFY the cause of the bradycardia.
Identification of the cause will determine the interventions that are implemented.
Symptomatic bradycardia in infants and children is usually the result of progressive respiratory failure or shock, which leads to tissue hypoxia and the resulting bradycardia.
Important note: In infants and children, cardiac output is primarily maintained through an increase in heart rate.
Remember: CO = stroke volume X HR
The ability to increase cardiac output by increasing stroke volume is limited in infants and children, and as a result, when bradycardia occurs, cardiac output will decrease.
Identification of the type of bradyarrhythmia present can help you determine its cause. The most common ECG rhythms classified as bradycardia include:
- Sinus Bradycardia
- First-degree AV block
- Second-degree AV block
- Type I —Wenckebach/Mobitz I
- Type II —Mobitz II
- Third-degree AV block complete block
Sinus Bradycardia:
Sinus bradycardia can be a normal response in a healthy child and will not be accompanied by symptoms (e.g., well-conditioned athlete). However, symptoms will be present when sinus bradycardia results from hypoxia, hypotension, and/or acidosis. This is why the assessment of the infant or child is critical for the identification and treatment of symptomatic sinus bradycardia.
AV Blocks:
AV blocks are caused by disrupting the electrical conduction system through the AV node. Some AV blocks may be present in healthy children. The identification of the specific AV block will help direct the care of the child. See the following pages for an overview of each specific AV block:
Intervene:
The initial interventions within the bradycardia algorithm for all infants and children with symptomatic bradycardia include the following:
- Identify and treat the underlying cause
- Provide oxygen
- Attach a cardiac monitor for rhythm identification
- Monitor blood pressure
- Monitor pulse oximetry
- Obtain IV or I/O access
- Obtain 12-lead ECG if possible
The above initial interventions are outlined in Step 1 of the Pediatric Bradycardia Algorithm.
After the initial interventions are implemented, the decision point for treatment within the bradycardia algorithm is the presence of cardiopulmonary compromise. (Step 2)
When the initial interventions carried out in Step 1 of the bradycardia algorithm fail to reverse symptomatic bradycardia and cardiopulmonary compromise with a heart rate < 60/min develops, CPR should be initiated. (Step 3)
When CPR is initiated in the infant or child with bradycardia and cardiopulmonary compromise, and this persists despite the interventions along with CPR, begin the administration of IV/IO epinephrine boluses. Atropine may also be considered in cases of bradycardia caused by increased vagal tone, cholinergic drug toxicity, or complete AV block. (Step 5)
When medications also fail to improve the situation, cardiac pacing (Step 5) may become necessary. Ensure that any potentially reversible causes of bradycardia are identified and treated, and use medications or cardiac pacing as a temporary means of cardiovascular support. In contrast, the underlying cause is identified, treated, and corrected.
Note: If dealing with primary bradycardia (defined above), atropine is preferred as the first-choice treatment of symptomatic AV block. If dealing with secondary bradycardia, atropine is not indicated for treating AV block, and epinephrine should be used.
Reversible causes and management of symptomatic bradycardia:
- Hypoxia
- Hydrogen ion (acidosis)
- Hyperkalemia
If pulseless arrest develops at any time during the treatment of bradycardia with cardiopulmonary compromise, implement the Cardiac Arrest Algorithm. (Step 6)
Bradycardia Diagram
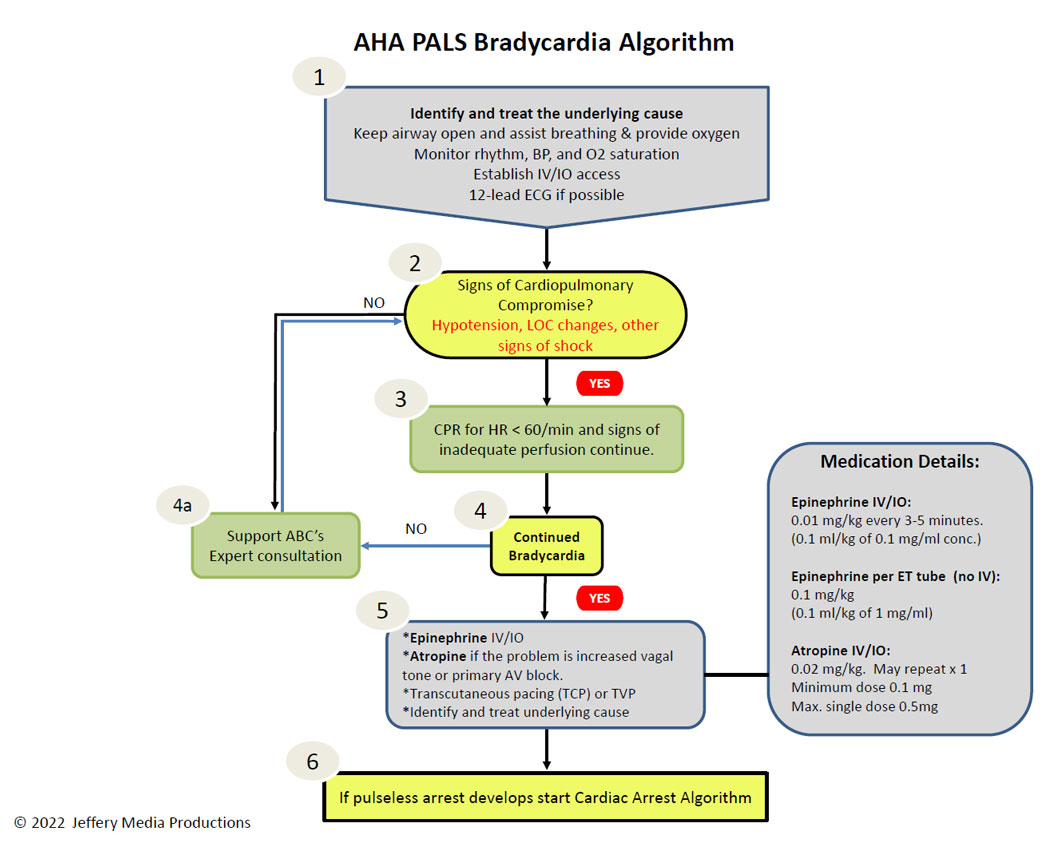
Members Download the Hi-Resolution PDF Here.
Austin says
What is the specific age for initiating compressions below 60bpm? All infants (below 1yr)?
ACLS says
Rather than a specific age the basic cut off is onset of puberty. This would be identifiable without having to know the specific age of a child in cardiac arrest or with symptomatic bradycardia.
Kind regards, Jeff
Joshua Jacobs says
What rate would we pace the child at? Do we adjust it based on the childs age? I would think a rate of 100bpm would work, increasing the mA until we saw electrical and mechanical capture. Would that be correct?
ACLS says
That is correct. You would adjust according to the minimum normal heart rate for the child’s age. You would start at the minimum obtain capture and then adjust the rate to improve clinical condition.
Kind regards,
Jeff
DR. MURTAZA KAMAL says
Good one for easy understanding
Galiwaxx says
In adults bradycardia is <60/min
So now between 9-16 yrs bradycardia is <50/min?
Jeff with admin. says
The numbers listed on the page above are a general reference for bradycardia in children. The specific definition is listed above those general guidelines. This is the definition of pediatric bradycardia: “A heart rate that is below the normal heart rate range for the childs age, level of activity, and clinical condition.”
Due to the variable nature of the heart rate in children, you must use the three indicators above to determine whether or not the patient has clinical bradycardia should be treated.
Kind regards,
Jeff